Last Updated on
The Ebola outbreak in Guinea, Liberia, and Sierra Leone continues. Being the most severe in recorded history – both in the number of cases and fatalities – a total of 1201 suspected cases with 672 deaths have been reported as of 23. July. Up-to-date information on the outbreak can be found under: ![]() Link
Link
A first case in Nigeria was reported by WHO on 25 July 2014: a Liberian man arriving at the city of Lagos by air on 20. July was hospitalised and later died of the disease. No secondary cases have been reported.
Starting in St. Martin in December last year, the epidemic has quickly expanded throughout the region (![]() Map). With almost all Carribean islands already affected and the first cases reported from Mexico (
Map). With almost all Carribean islands already affected and the first cases reported from Mexico (![]() Reference) and Venezuela (
Reference) and Venezuela (![]() Reference) it can be expected that the epidemic will continue to spread througout Central and South America. Additionally an autochthonous case of Chikungunya has been reported in Florida (
Reference) it can be expected that the epidemic will continue to spread througout Central and South America. Additionally an autochthonous case of Chikungunya has been reported in Florida (![]() Reference). Imported cases in travelers returning from the Carribean region are currently frequently seen in European countries and the number is very likely to increase.
Reference). Imported cases in travelers returning from the Carribean region are currently frequently seen in European countries and the number is very likely to increase.
New cases and deaths attributable to Ebola virus disease (EVD) continue to be reported by the Ministries of Health in the three West African countries of Guinea, Liberia, and Sierra Leone. Between 3 and 6 July 2014, 50 new cases of EVD, including 25 deaths, were reported from the three countries as follows: Guinea, 0 new cases and 2 deaths; Liberia, 16 new cases with 9 deaths; and Sierra Leone 34 new cases and 14 deaths. These numbers include laboratory-confirmed, probable, and suspect cases and deaths of EVD.
As of 6 July 2014, the cumulative number of cases attributed to EVD in the three countries stands at 844, including 518 deaths. The distribution and classification of the cases are as follows: Guinea, 408 cases (294 confirmed, 96 probable, and 18 suspected) and 307 deaths (195 confirmed, 96 probable, and 16 suspected); Liberia, 131 cases (63 confirmed, 30 probable, and 38 suspected) and 84 deaths (41 confirmed, 28 probable, and 15 suspected); and Sierra Leone, 305 cases (269 confirmed, 34 probable, and 2 suspected) and 127 deaths (114 confirmed, 11 probable, and 2 suspected). (![]() Reference)
Reference)
A laboratory-confirmed case of Crimean Congo Haemorrhagic Fever (CCHF) in a UK traveller who was bitten by a tick while on holiday in Bulgaria has been reported.
Background: CCHF is a primarily zoonotic virus infecting a wide range of domestic and wild animals. Domestic ruminant animals, such as cattle, sheep and goats, are viraemic for around one week after becoming infected. Humans are accidental hosts and get infected via tick bites. CCHF is endemic in Africa, the Balkans, the Middle East and in Asia south of the 50° parallel north, the geographic limit of the genus Hyalomma, the principal tick vector (![]() view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention. (
view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention. (![]() Reference)
Reference)
A major outbreak of chikungunya virus infection has been ongoing in the Caribbean since December 2013. The outbreak expanded also in Central and South America. There have been more than 280.000 probable and confirmed cases in the region. At least 22 fatalities have been reported so far.
Most of the areas previously involved continue to report increasing number of cases, and the situation is particularly severe in the island of Hispaniola island (Haiti and the Dominican Republic). El Salvador in Central America is still under a
declared national emergency with thousands of suspected cases. Several other countries have recently reported imported chikungunya infection in patients with travel history to the affected areas: Barbados, Bonaire, Brazil, Canada, Cayman islands, Chile, Cuba, France (including Tahiti), Grenada, Italy, Mexico, the Netherlands, Nicaragua, Paraguay, Panama, Peru, Spain, Switzerland, Trinidad and Tobago, Turks and Caicos Islands and many states in the USA. Costa Rica reported a confirmed case, but it is not clear if it is imported or autochthonous. Venezuela is reporting 12 cases, but it is not known if all are imported. (![]()
![]() Reference)
Reference)
Guinea
5. June 2014: cumulatively the total number of cases and deaths attributable to Ebola virus disease in Guinea is 351 (210 laboratory-confirmed, 83 probable, and 58 suspected) including 226 deaths. The geographical distribution of these cases and deaths is as follows: Conakry, 67 cases and 29 deaths; Gueckedou, 194 cases and 146 deaths; Macenta, 45 cases and 27 deaths; Dabola, 4 cases and 4 deaths; Kissidougou, 7 cases and 5 deaths; Dinguiraye, 1 case and 1 death; Telimele, 25 cases and 7 deaths; Boffa, 7 cases and 6 deaths; and Kouroussa, 1 case and 1 death. In terms of isolation, 33 patients are currently hospitalized (8 in Conakry, 9 in Gueckedou, 15 in Telimele, and 1 in Boffa). The number of contacts currently being followed-up countrywide is 1011.
Liberia
One suspected case from nearby Kailahun (Sierra Leone) died in Foya (Liberia). The dead body was taken back to Kailahun for burial. Eleven (11) contacts (5 health-care workers and 6 community relatives) were identified and are being followed up.
Sierra Leone
6. June 2014: 8 new cases (2 confirmed and 6 suspected) and 1 new death were reported from Kailahun This brings the total number of Ebola infections to 89 (33 confirmed, 3 probable, and 53 suspected) including 7 deaths. All 33 confirmed cases and 7 deaths were reported from Kailahun district. The number of cases among health-care workers is 5 and deaths is 1. There are currently 11 cases in isolation at Kenema Hospital. The number of contacts currently being followed-up is 30. (![]() Reference)
Reference)
17 autochthonous malaria cases have been reported from Aswan governorate in South Egypt since May [2014]. (![]() Reference)
Reference)
Egypt suffered from a malaria epidemic from 1942-1944, when around one million people were infected and 200.000 died. In 1942 the vector Anopheles gambiae was found in Egypt from the Sudanese border all the way up to 200 miles (300 km) south of Cairo in the Nile valley, but was pushed back by a larvicidal campaign which eradicated A. gambiae in Egypt and Sudan north of Khartoum. Studies are needed to determine the Anopheles species responsible for the present transmission in Aswan as well as active case detection to identify clinical cases and gametocyte carriers for treatment. (![]() Reference)
Reference)
On 27. May Iran reported its first two cases of MERS-CoV (Middle East respiratory syndrome coronavirus). Up to 23. May a total of 635 laboratory-confirmed cases of infection with MERS-CoV have officially been reported to the WHO, including 193 deaths (![]() Reference,
Reference, ![]() WHO). An excellent source of information on MERS-CoV:
WHO). An excellent source of information on MERS-CoV: ![]() link
link
A cholera outbreak has been reported from Alamada town, Cotabato province. Approx. 770 patients have been seeking medical care at hospitals (438 patients have been tested positive for Vibrio cholerae).(![]() References)
References)
Dominican Republic: 8034 cases reported. Currently 200 new cases per day. Mainly the South coast is affected. Cases are reported from 19 out of 31 Provinces (14.05.2014)
Haiti: Currently 14 confirmed cases. However, the minister of health cited 1529 cases (14.05.2014)
St. Martin / St. Maarten: St. Martin: first cases reported in december. Until now 3210 suspected cases, 793 confirmed cases, 3 fatal cases; St. Maarten: 123 confirmed cases on the dutch side of the island (04.05.14)
Martinique: 1515 confirmed and 21820 suspected cases (11.05.2014)
Guadeloupe: 1328 confirmed and 10600 suspected cases (11.05.2014)
St. Barthelemy: 135 confirmed and 490 suspected cases (11.05.2014)
British Virgin Islands: 20 confirmed cases (11.05.2014)
Dominica: 105 confirmed and 1252 suspected cases (26.04.2014)
Anguilla: 33 confirmed cases (06.04.2014)
St. Kitts and Nevis: First cases have been reported (22.03.2014)
St. Lucia: 5 confirmed and 25 suspected cases (14.05.2014)
St. Vincent: 3 confirmed and 36 suspected cases. Until now only the Island of Bequia appears to be affected (14.05.2014)
Antigua: 4 confirmed cases (14.05.2014) (![]() Reference)
Reference)
The French Ministry of Health has just alerted health professionals about the transmission of schistosomiasis in Corsica. At least 8 cases of S. haematobium schistosomiasis were diagnosed by the department of Parasitology of the Toulouse hospital. The cases were acquired after a bath in the Cavu/Cavo river close to the city of Porto Veccio in the South of the island, probably in 2011. (Personal communication)
As of 3. May 2014, the Ministry of Health (MOH) of Guinea has reported a cumulative total of 231 clinical cases of Ebola virus disease, including 155 deaths. There has been no change in the number of cases confirmed by ebolavirus PCR (127 cases) since the last update of 2 May 2014, but 1 additional death has been reported among confirmed cases (82 deaths). (![]() Reference)
Reference)
An outbreak of African sleeping sickness (African trypanosomiasis) has been reported in Rufunsa District in Lusaka Province. The Times of Zambia reports that 8 cases have been recorded at Mupanshya Hospital. The outbreak has been linked to an increase in the Tse-tse fly population mainly in the areas that border the Game Management Areas (GMAs). An increase in malaria cases has been observed in the same area. (![]() Reference)
Reference)
The CDC announced the 1st case of Middle East respiratory syndrome coronavirus infection (MERS) diagnosed in a Saudi Arabian traveler visisting the US. On 24. April 2014, the patient traveled by plane from Riyadh, Saudi Arabia to London, England then from London to Chicago, Illinois. The patient then took a bus from Chicago to Indiana. On 27. April 2014, the patient began to experience respiratory symptoms, including shortness of breath, coughing, and fever. The patient went to an emergency department in an Indiana hospital on 28. April 2014 and was admitted on that same day. Because of the patient’s symptoms and travel history, he was tested for MERS-CoV, which was laboratory confirmed on 2. May 2014. (![]() Reference)
Reference)
As of 23 April, the Ministry of Health of Guinea has reported a cumulative total of 218 clinical cases of Ebola Virus Disease, including 141 deaths (case fatality rate 65%). To date, 191 patients have been tested for ebolavirus infection and 115 cases have been laboratory confirmed, including 72 deaths. Twenty-six (26) health care workers (HCW) have been affected (18 confirmed), with 16 deaths (12 confirmed). Clinical cases of EVD have been reported from Conakry (58 cases, including 24 deaths), Guekedou (127/91), Macenta (22/16), Kissidougou (6/5), Dabola (4/4) and Djingaraye (1/1). Laboratory confirmed cases and deaths have been reported from Conakry (37 cases, including 19 deaths), Guekedou (63/41), Macenta (13/10), Kissidougou (1/1) and Dabola (1/1). The date of onset of the most recent clinical case, a suspected case, is 23 April while the date of isolation of the most recent confirmed case is 22 April. Overall, the epidemiological situation in Guinea has improved significantly over the last few weeks. The date of onset of the last reported case from Macenta was 24 days ago and a similar time has elapsed for Dabola (25 days), Kissigougou (26) and Djingaraye (31 days). Two incubation periods (42 days) without cases is the standard for declaring an EVD outbreak over in a particular location. (![]() Reference)
Reference)
Since April 2012, 370 laboratory-confirmed cases, including 113 deaths, of acute respiratory disease caused by Middle East respiratory syndrome coronavirus (MERS-CoV), have been reported by national health authorities. To date, all cases have either occurred in the Middle East, have had direct links to a primary case infected in the Middle East, or have returned from this area. The median age of the patients was ~50 years and 65% of the patients had an underlying chronic health condition. The source of the virus remains unknown but the pattern of transmission points towards an animal reservoir (see posting from 3. March 2014 below) in the Middle East, from which humans sporadically become infected through zoonotic transmission. Human-to-human transmission to close contacts and in hospital settings has occurred, but there is no evidence of sustained transmission among humans. MERS-CoV is genetically distinct from the coronavirus that caused the SARS outbreak. (![]()
![]() Reference)
Reference)
Guinea
As of 14 April, Guinea has reported a cumulative total of 168 clinically compatible cases of Ebola virus disease (EVD), including 108 deaths. Six districts of Guinea have reported patients – Conakry (31 patients, 22 laboratory confirmed), Guekedou (95 cases/35 confirmed), Macenta (21 cases/12 confirmed), Kissidougou (6 cases/1 confirmed), Dabola (5 cases/1 confirmed) and Djingaraye (1 suspected case). The date of onset of the most recently identified suspected clinical cases in Conakry and Guekedou was 10 April. One additional health care worker (HCW) has been reported, bringing the total to 16 (11 laboratory confirmed and 5 probable cases).
Liberia
As of 11 April, Liberia has reported a cumulative total of 26 clinical cases of EVD (6 laboratory confirmed, and 20 probable and suspected cases of EVD), including 13 deaths.
Mali
As of 14 April, Mali has reported a cumulative total of 6 suspected cases, all of whom remain under medical observation (3 in the capital city of Bamako, and 2 in Kourémalé and 1 in Bankoumana in the Koulikoro Region). The results of testing on these patients at the Institut Pasteur laboratory in Dakar, Senegal, are expected shortly.
(![]() Reference)
Reference)
Two male Dutch patients presented on 10. Mar. 2014 at the Center for Tropical and Travel Medicine of the Academic Medical Center in Amsterdam. Seven days after return from a holiday in the Philippines (5.-20. February 2014) they developed painful paresthesias on thorax and limbs. There were no visible skin lesions. Both patients were HIV positive, but had undetectable viral loads on antiretroviral treatment with stable CD4-counts greater than 500 x 10E6/l. On laboratory examination, serum eosinophilia (1.26 x 10E9/l and 0.66 x 10E9/l, respectively) was noted. Three days after presentation at our clinic, one patient developed a confused state and diplopia due to paralysis of the abducens nerve. CSF analysis showed an increased opening pressure, pleiocytosis and increased protein, but no increased eosinophil count. Empirical treatment for bacterial and herpes virus meningitis was initiated. Both bacterial cultures and PCR-analysis of the CSF were negative. A 2nd CSF analysis 5 days later did show an increased eosinophil count. With this clinical syndrome of eosinophilic meningo-encephalitis, a parasitic infection with Angiostrongylus sp. was suspected and treatment was started with prednisone and albendazole. PCR for Angiostrongylus sp. turned out to be positive in both patients, who are currently recovering. Both had been exposed by food consumption (salads, vegetables, shrimp, fish) in the Philippines. (![]() Reference)
Reference)
The Ministry of Health of Guinea has reported a cumulative total of 143 clinically compatible cases of Ebola virus disease (EVD), of which 54 are laboratory confirmed by PCR. The total number includes 86 deaths (CFR 60%). New cases have been reported from Conakry, Guekedou and Macenta; 23 patients are currently in isolation units. The current number of clinical and confirmed cases and deaths by place of report is Conakry (18 cases, including 5 deaths), Guekedou (85 cases/59 deaths), Macenta (27 cases/14 deaths), Kissidougou (9 cases/5 deaths), and Dabola and Djingaraye combined (4 cases/3 deaths). There has been no increase in the number of affected health care workers (HCW) from the 14 reported previously, including 8 deaths; 11 of the affected HCWs are laboratory confirmed cases. Sixteen of the 86 deaths overall are laboratory confirmed, 65 are classified as probable cases and 5 as suspected cases.(![]() Reference)
Reference)
The CDC and the Minnesota Department of Health have confirmed a diagnosis of Lassa fever in a person returning to the United States from West Africa. The patient was admitted to a hospital in Minnesota on 31. March 2014 with symptoms of fever and confusion. Blood samples submitted to CDC tested positive for Lassa fever on 3. April 2014. The patient is recovering and is in stable condition. (![]() Reference) Note: between 1969 and 2014 approx. 34 cases of imported Lassa fever have been diagnosed in Europe, the United States, Israel and Japan. Almost all cases were physicians, nurses, aid workers, engineers, peacekeepers etc. returning from one of the endemic West African countries.
Reference) Note: between 1969 and 2014 approx. 34 cases of imported Lassa fever have been diagnosed in Europe, the United States, Israel and Japan. Almost all cases were physicians, nurses, aid workers, engineers, peacekeepers etc. returning from one of the endemic West African countries.
A man has died from rabies in a Paris regional hospital after visiting Mali. France has eradicated rabies on its territory, officials say. It is an extremely rare case for France, where the disease was officially eradicated in 2001. Officials did not explain how the man had caught rabies in Mali. There has been no case of rabies being contracted by humans in mainland France since 1923. Rabies has been diagnosed in about 20 patients in France since 1970, all of whom caught it abroad. The last death was in 2003. (![]() Reference)
Reference)
There are now 49 confirmed cases of zika virus infections in the Cook Islands and as many as 630 people are believed to have been infected from the mosquito-born disease. Last month health authorities first thought they were dealing with dengue fever but the laboratory test results confirmed zika virus as the causative agent. It is highly likely that the virus was imported from French Polynesia, where the disease is currently causing an larger outbreak (see posting from 24. January 2014 below)(![]() Reference)
Reference)
A total number of 28 cases of hepatitis A infection has been reported over the last few months in Norway. In almost half of this unusually high number of cases, the patients were found to have infected with hepatitis A virus while traveling abroad. The remaining half got infected in Norway, which worries the health authorities,
who are currently investigating whether there may be a common source of infection.
(![]() Reference)
Reference)
The number of cases of the currently ongoing Ebola outbreak in Guinea (see posting from 26. March 2014) has increased to 122 and 78 deaths since the declaration of this deadly epidemic. (![]() Reference)
Reference)
The mysterious febrile illness circulating since Februrary in the South-Eastern provinces bordering Liberia and Sierra Leone (Guekedou, Macenta, Nzerekorem, and Kissidougou) has now been confirmed to be an outbreak of Ebola. Three suspeced cases from the capital Conakry turned out to be negative for Ebola. Of the 87 reported (suspected) cases 61 have died. The responsible Ebola virus strain was identified as Zaire Ebolavirus, consistent with the high mortality rate observed (![]() Reference). A suspected case of Ebola in a Canadian traveler who just returned from Liberia and was hospitalized in Saskatoon, Canada turned out to be not Ebola (
Reference). A suspected case of Ebola in a Canadian traveler who just returned from Liberia and was hospitalized in Saskatoon, Canada turned out to be not Ebola (![]() Reference).
Reference).
One confirmed and 40 suspected cases of Zika virus infections have been reported on Easter Island. Easter Island, or Isla de Pascua, more than 2,000 miles from the Chilean coast is governed by Chile’s Valparaíso Region. To control the outbreak, Chile increased preventive measures against mosquito vectors. The virus has probably been imported by tourists from other vacation islands in the region where Zika virus is currently casing local outbreaks (New Caledonia, French Polynesia, Tahiti; see posting from 24. January below) (![]() Reference)
Reference)
According to the Department of Health of the Philippines, 1.163 cases of measles and a number of measles deaths were reported in the country from January 1 through January 11, 2014. Most of the cases are from the Metropolitan Manila, Calabarzon, and Central Luzon. Countries reporting cases in travelers returning from the Philippines include Australia, Canada, Japan, New Zealand, the United Kingdom, and United States. (![]() Reference)
Reference)
Since the first report in September 2012, Middle Eastern Respiratory Syndrom Coronavirus (MERS-CoV) has sickened 183 people and killed 80, most of them in Saudi Arabia. The median age of the patients was ~50 years and 65% of the patients had an underlying chronic health condition. Over the last year more and more evidence cumulated that camels are playing a role in the spread of the disease. It has been found that a large percentage of camels in the Middle East have antibodies against MERS in their blood, while other animals, such as goats and sheep, do not. Now new evidence of MERV-CoV infections in camels from Sudan and Ethiopia suggests that Africa, too, harbors the pathogen (![]() Reference). That means MERS may sicken more humans than previously thought. Researchers have also isolated MERS-CoV RNA from nose swabs of camels in Qatar, and it has been shown that the virus has circulated in Saudi Arabian camels for at least 2 decades (
Reference). That means MERS may sicken more humans than previously thought. Researchers have also isolated MERS-CoV RNA from nose swabs of camels in Qatar, and it has been shown that the virus has circulated in Saudi Arabian camels for at least 2 decades (![]() Reference)
Reference)
During the past week, 490 new cases of Chikungunya have been reported in the Caribbean. New confirmed cases were reported from the French part of Saint Martin (52), the Dutch part of the island (Sint Maarten, 5), Martinique (326), Saint Barthélemy (21) and Guadeloupe (81). Four additional cases were notified in Anguilla and one imported case was recorded in French Guyana. (see postings from 13. & 29. December 2013, 10. January 2014 and 11. February 2014 below) (![]() Reference)
Reference)
On Bali Island, the first cases of rabies in humans and dogs were confirmed in 2008 on Bukit Peninsula. Despite control efforts in 2008–2009, rabies spread across the island. In the following 3 years, >130 persons died from rabies, and >130,000 persons received post-exposure vaccination after dog bites. After implementation of a mass dog vaccination program, the number of cases started to decline significantly (2011:
24 cases ;2012: 8 cases). However, despite enormous efforts rabies continues to be a problem: On 4. January a 46-years old man and on 25 January a 7-years old boy died of rabies after suffering dog bites. (![]() Reference)
Reference)
Just published: `Chikungunya in the Americas´ (![]() Link to publication) provides a summary of the recently reported emergence of this viral disease in the Carribean region. (see postings from 13. and 29. December 2013 and 10. Janurary 2014 below)
Link to publication) provides a summary of the recently reported emergence of this viral disease in the Carribean region. (see postings from 13. and 29. December 2013 and 10. Janurary 2014 below)
The private IST Medical Scheme Clinic in Dar es Salaam reports an increase in dengue fever cases in Dar es Salaam city. 10 proven cases (with rapid antigen/antibody test kits) have been diagnosed, starting halfway through December 2013 and increasingly so in the last 2 weeks. Most of these patients are expatriate residents in Dar es Salaam.
In 2010 more than 60 cases had been seen at the IST Medical Scheme Clinic; before 2010, cases were only sporadically diagnosed in Tanzania. (![]() Reference)
Reference)
Tests at two wastewater treatment plants in northern China revealed the presence of multi-drug-resistant, New Delhi Metallo-beta-lactamase (NDM-1) producing bacteria. The researchers found significant levels of NDM-1 producing bacteria in the effluent released to the environment and even higher levels in dewatered sludge applied to soils. (![]() Reference)
Reference)
Background: Carbapenems are the preferred treatment for severe infections caused by multidrug-resistant Gram-negative bacteria producing an extended-spectrum beta-lactamase (ESBL). Therefore the increasing and rapid spread of mobile genetic elements that determine acquired resistance to carbapenems and all other beta-lactams in Enterobacteriaceae is of great concern. In 2008, the first case of a novel carbapenemase “New Delhi metallo-beta-lactamase 1” (NDM-1) has been recognised in a Swedish patient who was repatriated to Sweden from the Indian subcontinent. Since this first report, cases involving New Delhi metallo-beta-lactamase (NDM)-producing Enterobacteriaceae have been reported from every continent except Antarctica. Although medical care in the Indian subcontinent was associated with many early reports, recent cases have been described involving persons who traveled to endemic regions but were not hospitalized. The plasmid-carrying NDM is highly transmissible to other bacteria, and bacteria carrying NDM can colonize the gastrointestinal systems of humans for prolonged periods. If colonization or infection of returning travelers, medical tourists or repatriated patients is suspected isolation and early detection is the only way to prevent nosocomial spread. The emergence of these `super bugs´ over the recent years is alarming and considered a serious threat to public health all over the world.
The sale of fake yellow fever (YF) vaccination cards/certificates has been a recurring problem in Nigeria. In 2013, the Nigeria Ministry of Health replaced old cards with a new type in an attempt to prevent the sale of fake cards (see posting from 27. Aug. 2013 (Nigeria: Yellow fever vaccination card recognition) in the right column below). However, the sale of fake yellow fever vaccination cards to individuals who did not receive the vaccine continues to present a serious public health problem inside and outside Nigeria. Susceptible, unvaccinated individuals may contribute to a YF outbreak within the country. YF virus is endemic in Nigeria, and an unvaccinated, viremic individual with a fake card who becomes infected in Nigeria could carry YF virus to localities where vector mosquitoes are present and initiate an outbreak of this serious disease. Recently it was reported that a man carrying a fake yellow fever vaccination card was arrested at immigration at the Idi-Iroko border post. (![]() Reference)
Reference)
Norovirus outbreaks are a major threat for cruise ship passengers (including the crew). One of the worst outbreaks in the last 20 years has recently occurred aboard the `Explorer of the Seas´ where nearly 700 people got infected while cruising in the Carribean. The cruise ship returned to New Jersey early on Wednesday [29. January 2014]. It was not possible to identify the source of the outbreak.
(![]() Reference)
Reference)
The CDC provides excellent surveillance information on recent and current outbreaks of infectious diseases aboard cruise ships: ![]() Link.
Link.
The Peruvian Ministry of Health reported 2 confirmed cases (a 28-year-old man and a 25-year-old woman) of Hanta virus infection currently treated in the Santa Rosa Hospital in Lima. In addition a 3rd probable case has been reported from Cuzco: a 26-year-old man who is hospitalized at the intensive care unit of the Cuzco Regional Hospital. The 3 patients participated in a tourist group trip (of 8 people) to the city of Iquitos, including a guided visit to the Amazonian region of the Mamon River in the Punchana district of Maynas province. The route of this tourist circuit included a 2-night stay in a hostel that consisted of 24 bungalow-rooms with wooden walls and a thatched straw roof. (![]() Reference)
Reference)
Background: Hanta virus infections occur sporadically throughout the Americas. Hanta viruses in the Americas cause `Hanta pulmonary syndrome´ (HPS) characterized by severe respiratory symptoms. Various Hanta viruses have been identified in North and South America and are transmitted to humans by inhalation of aerosolized dried rodent excreta. Some of the South American Hanta viruses may be transmitted between humans in a nosocomial setting.
New Caledonia:
The government of New Caledonia reported the 1st indigenous infection with the Zika virus. The case was confirmed by the Pasteur Institute. The patient is a 76-year-old man living in Dumbea. This is the 1st time a person has been infected on the Caledonian territory. The other 26 cases reported so far have been imported from French Polynesia, where a outbreak is currently taking place. (![]() Reference)
Reference)
French Polynesia & Tahiti:
Currently a larger outbreak of Zika virus infections has been reported in the islands of French Polynesia and Tahiti. The total number of Zika virus infection cases in French Polynesia has increased from 333 confirmed cases and 6630 suspected cases on 9. January 2014 to 361 confirmed and 7156 suspected cases only 4 days later (13. January 2014).
Background:
Zika fever is an illness caused by a virus that spread through mosquito bites. It is closely related to dengue virus and causes a similar illness. Symptoms of Zika fever may include fever, headache, red eyes, rash, muscle aches, and joint pains. The illness is usually mild and lasts 4-7 days. There is no vaccine against Zika fever. Infections in returning travellers have been observed. Concerning the differential diagnosis and the serological cross reaction with Dengue fever please see posting from 27. December 2013 below. An review on Zika virus infections can be found under: ![]() LINK
LINK
From 2003 through 20. December 2013, 648 laboratory-confirmed human cases of avian influenza A(H5N1) virus infection have been officially reported to the WHO from 15 countries around the world. Of these cases, 384 died (Case fatality rate ~59%). Whenever influenza viruses are circulating in poultry, sporadic infections or small clusters of human cases are possible, especially in people exposed to infected household poultry or contaminated environments. However, the H5N1 virus does not currently appear to transmit easily among people. As such, the risk of community-level spread of this virus remains low. (![]() Reference)
Reference)
What is the risk of international spread of H5N1 virus by travellers?
The risk for travellers is considered to be very low. However, recently a fatal case of a traveller has been reported: a young Canadian woman (age: ~20s) died of a severe H5N1 infection on 3. January 2014 in Alberta, Canada after returing from a holiday trip to Beijing, China. (![]() Reference)
Reference)
Influenza A(H7N9) is one of a subgroup of influenza viruses that normally circulate among birds. In February 2013 human infections were reported from the Chinese east coast for the first time (see posting from 4. April 2013 below): The first cases were reported between February and May 2013 (n=133), then two cases were reported in July and August, and since October 2013 a second wave of human cases has been recorded (n=74 thus far). As yet, there is limited information about the scope of the disease the virus causes and about the source of exposure. However, most human cases report a history of exposure to birds or live poultry markets. The disease is of concern because most patients have been severely ill and the case fatality rate is considered to be around 33%. Information to date does not support sustained human-to-human transmission.
What is the risk of international spread of H7N9 virus by travellers?
There is no indication that international spread of this virus in humans or animals has occurred. Until the virus adapts itself for efficient human-to-human transmission, the risk of international spread of H7N9 virus by travellers is very low. (![]() Reference)
Reference)
An outbreak of chikungunya in the Caribbean region was reported from the French part of the island of Saint Martin on 5. December 2013. This is the first time that autochthonous transmission of the virus has been documented in the Americas. Since then, new chikungunya cases have been reported from several islands in the Caribbean. As of 9. January 2014, the following numbers of cases have been reported:
– 201 probable or confirmed cases in Saint Martin (FR);
– 2 confirmed cases in Saint Martin (NL);
– 48 probable or confirmed cases in Martinique;
– 25 probable or confirmed cases in Saint Barthelemy;
– 10 probable or confirmed cases including one imported case from Saint Martin in Guadeloupe;
– 1 confirmed case imported from Martinique in French Guiana.
Background: Chikungunya transmission was detected during an ongoing dengue outbreak in the Caribbean. Dengue and chikungunya viruses are transmitted by the same Aedes aegypti mosquito species. The naive population, the presence of an effective vector in the region, and the movement of people in and between islands are factors that make it likely the outbreak will continue to spread geographically and increase in numbers. Since the dengue outbreak is ongoing, clinicians and travel medicine clinics should remain vigilant regarding imported dengue and chikungunya cases from the Caribbean. (![]() Reference)
Reference)
A previously healthy 51-year-old woman sought treatment in a hospital in Berlin on 9. September 2013 after returning from travel to Japan (Honshu). Since 3. September 2013 she suffered from fever up to 40 degree celsius and nausea, followed by a maculopapular rash. 9 days before admission she had returned from a 2 weeks round trip (19.-31. August 2013) from Japan [with sites visited on the following dates in August 2013]:
19-21 Ueda
21-24 Fuefuki
24-25 Hiroshima
25-28 Kyoto
28-31 Tokyo
She reported several mosquito bites while grape picking in Fuefuki. She flew nonstop from Frankfurt (International Airport) to Tokyo (Narita International Airport) and [back the same way]. Among several other diseases, dengue fever was suspected, because of the clinical picture. Initially, the 1st serum sample collected 7 days after disease onset gave a positive result in the dengue virus (DENV) IgM and IgG antibody tests (IFA [indirect fluorescent antibody] and rapid test), as well as for DENV NS1 antigen (ELISA and rapid test) demonstrating an acute DENV infection of the patient. Real-Time RT-PCR for DENV RNA and generic flavivirus RT-PCR were negative. After one week in hospital the patient was discharged with a characterization of restitutio ad integrum [total recovery]. A follow-up serum sample was collected in December 2013, because this acute case of dengue fever imported from Japan was considered very unusual. This 2nd serum sample collected 110 days after disease onset revealed a significant DENV IgG titer decrease (IFA) and negative results for DENV NS1 antigen (ELISA and rapid test) and DENV IgM (IFA and rapid test), respectively.
This is the 1st laboratory confirmed case of DENV infection imported from Japan to Germany. Most likely, according to the patient’s activities and DENV incubation period, the infection was acquired in Japan. Thus, differential diagnosis in febrile returning travelers from Japan (Honshu) in late summer [2013] should include dengue fever. In addition, the autochthonous transmission of DENV in Japan should be further investigated to take adequate prevention measures early. (![]() Reference)
Reference)
Recently the first laboratory confirmed case of Chikungunya virus infection has been reported from the American region (see posting from 13. December 2013 below). Meanwhile the virus genome has been completely sequenced from clinical samples. It is a strain of Asian genotype, and therefore different from the one which caused the 2006 outbreak in Reunion Island and then spread throughout the Indian Ocean. Currently the National Reference Centre for Arboviruses (IRBA, Marseille, France) investigates the endemic situation of Chikungunya in the Carribean region:
– St. Martin: 66 confirmed, 14 probable, 167 suspected
– St. Barthélemy: 11 suspected;
– Guadeloupe: 1 confirmed, 21 suspected;
– Martinique: 3 confirmed, 27 suspected;
– Guyana: 1 confirmed (ex Martinique), no number given of suspected
(![]() Reference)
Reference)
A previously healthy 53-year-old man consulted at the Saarland University Medical Center on 22 Nov 2013 after returning from travel to Thailand. During his 3-week round trip (31 Oct-20 Nov 2013), including visits to Phuket, Krabi, Ko Jum, and Ko Lanta, he developed joint pain and swelling on his left ankle and foot on 12 Nov 2013 after several mosquito bites, followed by a maculopapular rash on his rear and front trunk that spread to the face and the upper as well as lower extremities over the next 4 days before fading. Accompanying symptoms were malaise, fever, and shivering, of which the latter 2 appeared only for one day.
Initially, the 1st serum sample collected 10 days after disease onset gave a positive result in the dengue IgM antibody tests (IFA and rapid test), although tests for dengue IgG antibody (IFA and rapid test) and dengue NS 1 antigen (ELISA and rapid test) were negative. However, the isolated positive result for dengue IgM antibodies prompted to investigate a probable flavivirus etiology through a serological approach. Serological tests for Japanese encephalitis virus, West Nile virus, Yellow fever virus, tick-borne encephalitis virus, and Zika virus were performed by the WHO Collaborating Centre for Arbovirus and Haemorrhagic Fever Reference and Research (WHOCC), Hamburg, Germany. IFAs gave positive results for Zika virus IgG and IgM antibodies, demonstrating an acute or recent Zika virus infection of the patient. In contrast, IFAs gave negative results for the other flaviviruses tested as well as for chikungunya virus. The presence of ZIKV-specific neutralizing antibodies was confirmed by a virus neutralization assay, and an IgM titer decrease in IFA was demonstrated in the 2nd serum sample collected 31 days after disease onset. This is the 1st laboratory confirmed case of ZIKV reported in Germany and Europe and the 2nd case reported from Thailand. Thus, differential diagnosis in febrile returning travelers from the south of Thailand (Phuket, Krabi, Ko Jum, and Ko Lanta) should include Zika virus infection. (![]() Reference) (also see posting below: 30. May 2013 – Canada ex Thailand: Zika virus in a returning Canadian traveler)
Reference) (also see posting below: 30. May 2013 – Canada ex Thailand: Zika virus in a returning Canadian traveler)
The WHO recently confirmed that a previously reported and unknown illness in Tanzania’s Kigoma Region (![]() map) is hepatitis E. 15 out of the 46 samples were tested positive for hepatitis E virus. Between August 20 and October 29, the region’s Buhigwe District experienced 690 acute febrile illness cases with no deaths. Most patients presented with vomiting, loss of appetite, generalized body weakness, abdominal pain, high fever and headache. A small proportion of the cases experienced diarrhea and jaundice. Approximately 61% of reported cases occurred in individuals below the age of 15 years. Approximately 54 percent of the cases occurred in females. (
map) is hepatitis E. 15 out of the 46 samples were tested positive for hepatitis E virus. Between August 20 and October 29, the region’s Buhigwe District experienced 690 acute febrile illness cases with no deaths. Most patients presented with vomiting, loss of appetite, generalized body weakness, abdominal pain, high fever and headache. A small proportion of the cases experienced diarrhea and jaundice. Approximately 61% of reported cases occurred in individuals below the age of 15 years. Approximately 54 percent of the cases occurred in females. (![]() Reference)
Reference)
On 6. December 2013, WHO was notified of 2 laboratory confirmed cases of locally acquired chikungunya disease in the French part of the Caribbean isle of Saint Martin (map). The other part of the isle is a country that is part of the Kingdom of the Netherlands (Sint Maarten). There has been an outbreak of dengue fever on St Martin / Sint Maarten since January 2013. Chikungunya disease was detected during an investigation following the notification of 5 cases with joint pains and fever on 18. November 2013, for whom the diagnosis of dengue was excluded. The onset of symptoms of the 5 cases occurred between 12. October and 15. November 2013. As of 10. December 2013, two confirmed, 4 probable and 20 suspected cases of chikungunya infection have been reported. This is the first time that locally acquired transmission of chikungunya has been detected in the American Region. (![]() Reference) (
Reference) (![]() Chikungunya risk map ,
Chikungunya risk map , ![]() Chikungunya factsheet)
Chikungunya factsheet)
One case of locally acquired Dengue fever has been reported from the department Bouches du Rhone (![]() map) in the South of France in November 2013. Southern France has an established population of Aedes albopictus mosquitoes, a competent vector for dengue and chikungunya viruses. Given the frequency of dengue cases imported into France (168 imported dengue cases in 17 departments in 2013), the risk of secondary cases is real. However, till now only two cases of autochthonous dengue transmission have been reported from the South of France in the past (
map) in the South of France in November 2013. Southern France has an established population of Aedes albopictus mosquitoes, a competent vector for dengue and chikungunya viruses. Given the frequency of dengue cases imported into France (168 imported dengue cases in 17 departments in 2013), the risk of secondary cases is real. However, till now only two cases of autochthonous dengue transmission have been reported from the South of France in the past (![]() Eurosurveillance 2010). (
Eurosurveillance 2010). (![]() Reference)
Reference)
The Food and Drug Administration of the Philippines has warned the public against a counterfeit rabies vaccine that is being sold in the country. The FDA and Novartis Healthcare (Philippines) have determined that there is an illegally imported and unregistered Purified Chick Embryo Cell (Rabipur) Rabies Vaccine being offered for sale in vaccination clinics, drug establishments and outlets, and internet websites. A complaint sample of the vaccine was collected at Tabuk City in Kalinga, and it was verified that the sample was counterfeit. (![]() Reference)
Reference)
Following a confirmed outbreak in French Polynesia, 2 cases of Zika fever have been reported in New Caledonia. Zika fever is a viral illness clinically similar to Dengue fever and is spread though mosquito bites. The islands in French Polynesia affected by the Zika virus outbreak this year (2013) are: Tahiti, Moorea, Raiatea, Tahaa, Bora Bora, Nuku Hiva, and Arutua. There was a major outbreak of Zika virus infections on Yap and nearby islands of the Federated Republic of Micronesia in 2007. New Caledonia has had an outbreak of Chikungunya virus infections this year (September 2013), and the mosquito vectors involved in that outbreak are competent vectors of Zika virus. (![]() Reference)
Reference)
Since the first report in September 2012, a total of 160 cases of MERS-CoV infection have been confirmed (including 68 fatal cases). The median age of the patients was 50 years, 64,5% were male and 65% of the patients had an underlying chronic health condition. Most cases have been reported from Saudi Arabia. (see earlier postings on MERV-CoV below)
Suffolk County Commissioner of Health Services James Tomarken announced Nov. 20 that his department had confirmed a case of locally acquired dengue in his county. The patient, a 50-year-old man, was hospitalized with dengue symptoms in Sept. and has now recovered. This is believed to be the first locally acquired dengue illness in New York State. He had no history of travel outside the region. (![]() Reference)
Reference)
A group of 10 travelers from Israel were infected with schistosomiasis after a single, brief freshwater exposure at Nyinambuga Crater Lake in Uganda [Kabarole District], where the altitude is 1630 meters. This outbreak proves that even at high altitude, Schistosoma mansoni may exist, despite previous studies claiming that there is protection from this disease at above 1400 meters. (![]() Reference)
Reference)
Researchers have identified a fifth dengue subtype, the first new subtype in 50 years, a finding that could add another challenge to vaccine development, according to findings presented at a dengue meeting under way in Bangkok. The subtype was identified during screening tests on virus samples that were collected during an outbreak in Malaysia in 2007. The findings were presented by Nikos Vasilakis, PhD, lead author of the study and a virologist from the University of Texas Medical Branch (UTMB) in Galveston. The researchers’ analysis suggested that the virus was different from the current four subtypes, and their sequencing tests found that it was phylogenetically distinct. Tests on monkeys found that the virus provoked different antibodies than for the other four subtypes. (![]() Reference)
Reference)
Just published: Malaria tropica in travelers is almost exclusively diagnosed within two months after returning from an endemic country. The authors present a male patient (immigrant) with severe P. falciparum malaria diagnosed 2.5 years after returning from Burkina-Faso. The authors speculate that their patient was chronically infected with P. falciparum malaria for more than 2 years, with an undetectable parasite index and without symptoms. Because of waning immunity clinically overt P. falciparum malaria was able to develop. This case illustrates the importance of malaria suspicion as a cause of illness in immigrants from malaria-endemic countries. Even when these immigrants did not travel for a long time, malaria should be considered in patients with typical symptoms. (![]() Reference)
Reference)
The WHO has been informed of an additional laboratory-confirmed case of Middle East respiratory syndrome coronavirus (MERS-CoV) infection in Qatar. The patient is a 23-year-old man who was identified as a close contact of a previously laboratory-confirmed case as part of the epidemiological investigation. He is a worker in the animal barn owned by the previously laboratory-confirmed case. The man developed mild symptoms of illness and is in good condition. Preliminary investigations revealed that he did not recently travel outside the country. Globally, from September 2012 to date, WHO has been informed of a total of 145 laboratory-confirmed cases of infection with MERS-CoV, including 62 deaths. (![]() Reference)
Reference)
The WHO has confirmed 10 polio cases in north-east Syria, the first confirmed outbreak in the country in 14 years, and warned that the disease could spread across the region. Officials are awaiting laboratory results on another 12 cases that presented with polio-like symptoms. (![]() Reference)
Reference)
There have been several cases of poisoning in Indonesia from alcoholic drinks adulterated with harmful substances, particularly methanol. Locals and foreigners have died or have become seriously ill mostly in the islands of Bali and Lombok. In August 2013 15 fatal cases of methanol poisioning have been reported in Indonesia, including a German and a British tourist. Over the years 22 cases of methanol poisoning in tourists have been published. Cases have usually involved local spirits (such as rice-based arak) and cocktails, but brand name alcohol can also be adulterated.
Just published: a case of P. knowlesi malaria has been reported in a tourist returning from Thailand (most likely acquired in Ranong / Khao Sok National Park). To date only 5 cases of imported P. knowlesi malaria have been observed in returning European travelers (Sweden ex Malaysia-Borneo, Finnland ex Malaysia-Peninsula, Spain ex Southeast Asia, France ex Thailand-Kho Phayam). (![]() Reference)
Reference)
28 cases of hepatitis A have been confirmed in Ashburton, Methven and Rakaia since April 2013. The outbreak has been traced to an asymptomatic infection in a young child of a family who had traveled overseas without vaccination against hepatitis A. (![]() Reference)
Reference)
Madagascar had 256 plague cases and 60 deaths last year, the world’s highest recorded number. The number of cases rises each October as hot humid weather attracts fleas, which transmit the disease from rats and other animals to humans. (More than 90% of the worldwide recorded cases of plague are reported from Madagascar and Congo DRC). (![]() Reference)
Reference)
From 9. September to 13. October 2013 a total of 159 cholera cases have been recorded in Mexico (V. cholerae O1, Ogawa): 145 cases in Hidalgo, 2 cases in the Ferderal District (Mexico city), 9 cases in Mexico state, 1 case in San Luis potosi, 2 cases in Veracruz state. It is the first time since 2001 that autochthonous cases of cholera are recorded in Mexico. The identified cholera strains are identic to the ones isolated in Haiti.
Sarawak, Malaysia: A total of 7358 cases of hand-foot-mouth disease (HFMD) have been recorded in the state from the beginning of the year till 21. September 2013. According to national statistics there were 11903 cases during the corresponding period last year [2012]. Kuching Division registered the most cases (1737), followed by Miri (1712 cases), Sibu (1022 cases), Samarahan (550 cases), Sarikei (487 cases), Limbang (387 cases), Bintulu (369 cases), Mukah (346 cases), Kapit (309 cases), Sri Aman (222 cases), and Betong (217 cases).
Hong Kong, China: The number of cases of hand, foot and mouth disease rose dramatically in the 1st 9 months of this year, and more adults are getting sick. More than 4200 cases of the disease were reported in the city, overtaking the total of the previous 2 years combined [2011-2012]. The viral infection mainly affects children, but doctors have recently been seeing more cases in adults.Year / no. of cases:2008 / 9672009 / 7272010 / 50252011 / 13702012 / 22162013 / 4256 (as of 2. October 2013)
After the death of a man from Rocky Mountain spotted fever in August, the Prefecture of Tombos, Zona da Mata, Minas Gerais has installed 2 warning signs about suspected star tick infestation on the Carangola river. Over the past 6 years, 66 cases of the disease were confirmed in Minas Gerais.
Background: Rocky Mountain spotted fever is a rickettsial disease prevalent throughout the Americas (and the most lethal and most frequently reported rickettsial illness in the United States). Some synonyms for Rocky Mountain spotted fever in other countries include `tick typhus´, `Tobia fever´ (Colombia), `São Paulo fever´ or `febre maculosa´ (Brazil), and `fiebre manchada´ (Mexico). The disease is caused by the bacterium Rickettsia rickettsii, which is spread to humans by the bites of Dermacentor ticks. Initial signs and symptoms of the disease include sudden onset of fever, headache, and muscle pain, followed by development of rash. The disease can be difficult to diagnose in the early stages, and without prompt and appropriate treatment it can be fatal. (![]() Reference)
Reference)
A total number of 107 imported Chikungunya fever cases have been reported in Australia, which indicates a significant increase in the number of cases compared with the previous years (year – number of cases): 2012 – 19 / 2011 – 37 / 2010 – 53 / 2009 – 28 / 2008 – 12 / 2007 – 1 / 2006 – 3 / 2005 – 0 (![]() Reference)
Reference)
The multistate hepatitis A outbreak linked to ‘Townsend Farms Organic Antioxidant Blend’ (see previous posting from 20. June 2013 below), which contained pomegranate seeds from a company in Turkey, has increased to 162 cases as of 20. September 2013. The cases have been recorded from 10 states to include Arizona (23), California (79), Colorado (28), Hawaii (8), New Hampshire (1), New Jersey (1), New Mexico (11), Nevada (6), Utah (3), and Wisconsin (2). The CDC notes that the cases reported from Wisconsin resulted from exposure to the product in California, and the cases reported from New Hampshire reported fruit exposure during travel to Nevada. All those affected reported eating this product purchased it from Costco markets. (![]() Reference)
Reference)
As of 12 September 2013, 139 human cases of West Nile fever were reported in the EU and 289 cases of West Nile fever in neighboring countries since the start of the 2013 transmission season. With 33 new cases detected in the European region in the last week the number of cases are currently peaking and new regions have been reached by the virus, including 4 newly affected provinces in Italy (Verona, Reggio Emilia, Mantova and Bologna) and 2 newly affected counties in Romania (Tulcea and Constanta). (A reported case from Austria was withdrawn when additional laboratory tests found no West Nile virus infection). (up-to-date figures can be found by following the link `West Nile fever surveillance Europe´ on the right side of this webpage)
Currently TropNet member sites report an sharp increase in travelers diagnosed with typhoid fever after returning from summer holidays (July-August) in Nepal.
Florida health officials have issued a health alert Friday as the number of confirmed cases of Dengue fever rose to 12. One new case was just reported in Miami-Dade county, the others were in Martin and St. Lucie counties.
Background: See posting from 26. August 2013 below. In 2009, a Key West outbreak affected 28 people. Until then, no cases of dengue had been seen in Florida for 40 years. (![]() Reference)
Reference)
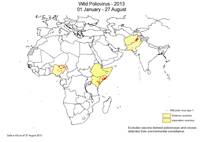
Wild poliovirus (WPV) cases
Total cases: Year-to-date 2013 / Year-to-date 2012 / Total 2012
Globally: 214 / 128 / 223
– in endemic countries: 72 / 123 / 217
– in non-endemic countries: 142 / 5 / 6
Current issues:
– The outbreak of wild poliovirus type 1 (WPV1) in the Horn of Africa, which affects Somalia, Kenya and Ethiopia (see posting from 14. June 2013), has spread into 2 new states of Somalia.
– In Israel, the number of sewage samples which have tested positive for WPV1 has reached 85; one sewage sample collected in West Bank and Gaza has tested positive for WPV1. (see posting from 14. June 2013) (![]() Reference)
Reference)

Nigeria’s Minister of Health, has urged travellers who are still using old yellow fever vaccination cards/certificates to replace it with the new encoded one (WHO-![]() International Certificate of Vaccination or Prophylaxis). Nigeria has announced not to recognise old cards/certificates any longer starting 1. October 2013 . (
International Certificate of Vaccination or Prophylaxis). Nigeria has announced not to recognise old cards/certificates any longer starting 1. October 2013 . (![]() Reference)
Reference)
The Florida Department of Health in Miami-Dade, Epidemiology, Disease Control and Immunization Services (EDC-IS) confirmed a case of dengue 4 virus in an 18-year old male with no recent travel history outside the United States as well as a recently confirmed imported case of dengue 4 virus in 56-year old male. Upon further investigation, it was identified that the two cases reside in the same household. (![]()
![]() Reference)
Reference)
Rabies has been confirmed in a man who was bitten by a dog in the streets of Valpariso on 17. July 2013. Chile has been free of terrestrial rabies for the last 20 years. (![]() Reference)
Reference)
On 24. July 2013 cholera has been confirmed in a 47 year old Italian male patient, who had traveled to Havana from 23. June to 13. July 2013. (![]() Reference)
Reference)
Background: Between late July and early August 2013, four additional cases of imported cholera in travelers have been reported: two cases of cholera were reported from Venezuela (a 51 year old male and 55 year old female patient who recently had travelled to Havana) and two cases were reported from Chile (both persons had returned from travelling to Cuba).
Currently two cholera outbreaks are ongoing in the Americas: Haiti and Cuba.
Haiti: since the beginning of the epidemic (October 2010) to epidemiological week (EW) 32 of 2013, the total number of cholera cases reached 669.645, of which 371.099 were hospitalized and 8.224 died. The global case-fatality rate has been 1.2% since November 2011, however, with variations for example in Sud Est (4.5%) and Port-au-Prince (0.6%).
Cuba: in early 2013, there were 51 confirmed cases of cholera in an outbreak in Havana, related to food handling. Previously, a total of 47 cholera cases had been reported, following Hurricane Sandy, in the provinces of Camaguey, Guantanamo and Santiago de Cuba. All cases were characterized as Vibrio cholerae toxigenic serogroup O1, serotype Ogawa, biotype El Tor.
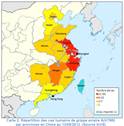
Up to 11. August 2013 a total of 135 cases (including 45 fatal cases; case fatality rate 33%) of H7N9 avian influenza have been confirmed on the Chinese mainland. The first human case of H7N9 avian influenza had been reported in late March 2013 (see postings from 1., 4., 12., 13., 17., 25. April 2013), with most cases confined to eastern China, and only one reported outside the mainland, in Taiwan. Unlike N5N1 avian influenza H7N9 appears to spread more easily and possibly mainly by the fecal-oral route. (![]() Reference)
Reference)
Most human rabies cases are reported from densely populated States/Divisions such as Ayeyarwaddy, Bago, Mandalay, Magway, Mon, Sagaing, and Yangon. A 2003 survey estimates that the dog population in Myanmar is approximately 3.48 million, and dog vaccination coverage is less than 1% with 98.2% of human rabies cases being related to dog bites. An estimated 600.000 persons are exposed to dog-bites each year. Approximately 200 human rabies cases are reported annually but it is estimated that the total number of human rabies cases exceeds 1000. (![]()
![]() Reference)
Reference)
Just published: A marked increase in the number of multidrug-resistant (MDR) tuberculosis (TB) cases entirely related to patients born in the Former Soviet Union was observed in France in the last two years. Very few cases were clustered, suggesting it is a consequence of recent immigration of patients already infected in their country of origin. This major increase challenges the existing structures for management of MDR and extensively drug-resistant TB (XDR-TB). (![]() Reference)
Reference)
Three fatal cases of an hemorrhagic fever have been reported from northern Uganda. Initally an outbreak of Ebola or Marburg hemorrhagic fever has been suspected. Now Crimean-Congo hemorrhagic fever (CCHF) has been confirmed in a survivor who is currently treated at Kalongo Hospital in Agago district, 450 km north of the capital Kampala. Uganda has suffered several episodes of Ebola and Marburg hemorrhagic fever since 2000. Last year two outbreaks of Ebola and one outbreak of Marburg have hit the country (see postings from 17. January 2013 and 14. October 2012 below) (![]() Reference).
Reference).
Background: CCHF is a primarily zoonotic virus infecting a wide range of domestic and wild animals. Domestic ruminant animals, such as cattle, sheep and goats, are viraemic for around one week after becoming infected. Humans are accidental hosts and get infected via tick bites. CCHF is endemic in Africa, the Balkans, the Middle East and in Asia south of the 50° parallel north, the geographic limit of the genus Hyalomma, the principal tick vector (![]() view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention.
view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention.
The Ministry of Health, Labour and Welfare said on Thursday [15. August 2013] that Japan has confirmed its first blood donor who was screened positive for Chagas disease.The blood donor, a man from Latin America was tested positive for Chagas disease after he has already donated blood 10 times from 2006 to June 2013. The Ministry of Health, Labour and Welfare and the Japanese Red Cross Society are currently trying to locate the recipients of the donated blood. The Japan Red Cross handles all blood donations in Japan. Since 15. October 2012 a voluntary declaration of living or traveling to Latin American countries has been implemented for blood donors. The declaration of the now positive tested blood donor was obtained in June 2013, but not for the previous 9 donations. (Reference)
An increasing number of returning travelers import typhoid fever to Australia. Many of the cases are Australians of Indian descent returning from visiting friends and family on the Indian subcontinent. The number of cases reported to the Department of Health has doubled in the past 5 years. Before 2007, there were 50 to 70 cases a year. In 2008, 100 were reported. There were 135 in 2011, 123 in 2012, and there have been 101 cases so far in 2013. There were 32 in January alone. (![]() Reference)
Reference)
Just published: the first ever recorded outbreak of carbapenem-resistant NDM-1-producing Acinetobacter baumannii in Europe has just been published. The case cluster occured in a French intensive-care unit in January to May 2013. The index patient was transferred from Algeria and led to the infection/colonisation of five additional patients. Concurrently, another imported case from Algeria was identified. The seven isolates were genetically indistinguishable. (![]() Reference)
Reference)
In Europe, the dynamics of endemic hepatitis E virus (HEV) infection remain enigmatic. Now a Dutch study provides new insights: Using blood donations collected throughout the Netherlands in 2011 and 2012, 40.176 donations were tested for HEV-RNA. The screening identified 13 viraemic donors and showed a HEV-IgG-seroprevalence ranging from 13% among donors younger than 30 years to 43% in donors older than 60 years. The finding of 17 HEV-RNA-positive donations among 45.415 donations corresponds to one HEV-positive blood donation per day in the Netherlands. For 16 of the 17 HEV-RNA-positive donors, genotyping succeeded, revealing HEV genotype 3, which is circulating among Dutch pigs. Apparently, clinically silent HEV infection is common in the Netherlands, which possibly applies to larger parts of Europe. (![]() Reference)
Reference)
The Saudi Arabian Ministry of Health reports 3 newly detected cases of the novel coronavirus (MERS-CoV) infection. A 67-year-old female citizen from Riyadh, who has various underlying chronic conditions (and who is currently hospitalized in intensive care) and two 39-year-old female health care workers (one in Asir and the other one in Riyadh). Both health care workers have only mild symptoms and their conditions are stable. As previously seen, it appears that serious clinical disease is mostly seen in infected individuals having pre-existing co-morbidities, whereas previously healthy individuals without pre-existing co-morbidities show milder clinical disease. These 3 newly reported, confirmed cases of MERS-CoV infection are raising the global case count to 94 including 46 deaths. As of 1. August 2013, the number of confirmed cases in Saudi Arabia is now 74 including 39 deaths. (![]() Reference)
Reference)
The polio outbreak in the Horn of Africa region (see posting from 28. June 2013) is expanding, with 21 newly-reported cases (1 from Kenya, 20 from Somalia). In Somalia, two immunization campaigns have been conducted since the most recent case occurred. (![]() Reference)
Reference)
The 1st rabies outbreak in Bali occurred in 2008 in Ungasan village. Since then, Bali has gone through 3 stages of mass vaccinations for dogs, monkeys and cats, all of which are believed to be rabies carriers. This year, from April to July 2013, the 4th stage of the mass vaccination is taking place, targeting inoculating 250.000 of the 350.000 dog population.
Rabies cases in humans in Bali have been decreasing in recent years, thanks to the mass animal vaccination initiative. In 2008, 4 cases were recorded, while 2009 saw 48 cases. The largest number, 82 cases, was recorded in 2010. After the mass animal vaccination program was launched in Bali, rabies cases in humans started to decrease. In 2011, 24 cases were recorded, and by 2012, only 8 cases had occurred.
Vaccinations for humans are performed in 33 rabies centers housed in community health centers, Sanglah Hospital, and 9 regional hospitals free of charge. (![]() Reference)
Reference)
Chikungunya outbreaks continue to pop up around various Philippines islands this year. Now 56 cases of chikungunya fever have been reported in Negros Occidental (![]() map) (50 in Kabankalan City and 6 in Cadiz City). (
map) (50 in Kabankalan City and 6 in Cadiz City). (![]() Reference)
Reference)

7 fatal cases of Crimean-Congo hemorrhagic fever (CCHF) have been reported in Amreli district, Gujarat province over the last week while 6 others are undergoing treatment. (![]() Reference)
Reference)
Background: CCHF is a primarily zoonotic virus infecting a wide range of domestic and wild animals. Domestic ruminant animals, such as cattle, sheep and goats, are viraemic for around one week after becoming infected. Humans are accidental hosts and get infected via tick bites. CCHF is endemic in Africa, the Balkans, the Middle East and in Asia south of the 50° parallel north, the geographic limit of the genus Hyalomma, the principal tick vector (![]() view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention.
view map). CCHF outbreaks constitute a threat to public health services because of its epidemic potential, the high case fatality rate (10-40%), the potential for nosocomial outbreaks and the difficulties in treatment and prevention.
Due to the current situation with persistent reporting of novel coronavirus (MERS-COV) infections in the Middle East, the Saudi Arabian Ministry of Health has published a recommendation to postpone participation in Umrah and Hajj this year if the pilgrim belongs to one of the following risk groups: elderly and people with chronic diseases (such as chronic heart, kidney, or pulmonary disease and diabetes mellitus), patients with congenital and acquired immunedeficiency, patients with malignancies, pregnant women and children. (![]() Reference)
Reference)
14. July: The Ministry of Health in the United Arab Emirates (UAE) has notified the WHO of a laboratory-confirmed case of infection with Middle East respiratory syndrome coronavirus (MERS-CoV) in the country. The patient is an 82-year-old man with underlying medical conditions and is currently in critical condition
11. July: The Ministry of Health in Saudi Arabia has reported an additional laboratory-confirmed case of Middle East respiratory syndrome coronavirus (MERS-CoV) infection in the country. The patient is a 66 year-old man from Asir region with an underlying health condition. He is currently in critical but stable condition.
Globally, from September 2012 to date, WHO has been informed of a total of 82 laboratory-confirmed cases of infection with MERS-CoV, including 45 deaths. (![]() Reference) (also see posting from 17. June 2013 below)
Reference) (also see posting from 17. June 2013 below)
The U.S. Embassy, Pristina advises U.S. citizens that Kosovo is experiencing a cyclical outbreak of Crimean-Congo hemorrhagic fever (CCHF), which is endemic to this area. National Institute of Public Health of Kosovo (NIPH) has recently reported 5 fatal cases of CCHF in the Malisheva/Malishevo, Rahovec/Orahovac and Gjakova/Gjakovica municipalities. Those most at risk are individuals with contact with livestock in endemic regions. (![]() Reference) (for information on CCHF see posting from 15. Jan. 2013)
Reference) (for information on CCHF see posting from 15. Jan. 2013)
The EpiSouth network published an extensive summary of the West Nile Virus (WNF) circulation in the European region and the neighbouring areas for the seasons 2010, 2011 and 2012. ![]()
![]() report.
report.
Polio has paralyzed 25 children in Somalia and another 6 in a Kenyan refugee camp since early May 2013. Before this outbreak, no polio cases were reported from Somalia for more than 5 years. There were only 223 polio cases around the world in 2012, the lowest ever recorded. Even in the remaining 3 endemic countries – Afghanistan, Pakistan and Nigeria – polio was only showing up isolated in a few remote areas. There have been 77 polio cases reported worldwide so far this year, compared with 84 to this point in 2012. But almost half of this year’s cases have occurred in Somalia and Kenya. Political instability prevents polio eradication in the last endemic regions. (![]() Reference)
Reference)
On 6. May 2013, the patient (male, 52 years) was bitten on his right hand by a small dog on a compound in Port-au-Prince, Haiti. He had cleaned the bleeding wound with water and alcohol. He had not been vaccinated against rabies before the accident and had not sought medical attention afterwards.
On 19. June 2013 (34 days after the bite), he developed fever and malaise, with headache and a painful right arm. Upon touch, he had dysaesthesia on his right arm and shoulder and on the right side of the trunk. On 20. June 2013, he developed hydrophobia and one day later, he developed swallowing problems, with reflex vomiting upon attempting to drink. He was admitted to a local hospital (Diakonessenhuis Utrecht, The Netherlands), where the attending neurologist suspected rabies. He was then transferred to our hospital (Academic Medical Center Amsterdam). Presence of rabies virus (genotype 1) was confirmed in skin biopsies of the neck, CSF and saliva. He is currently treated at the intensive care unit of the AMC in Amsterdam, according to a ‘modified’ Milwaukee protocol (rabies immunoglobulin, i.v. ribavirin, and hypothermia).(![]() Reference)
Reference)
The multistate hepatitis A outbreak associated with frozen berries sold at Costco (see postings from 3. June 2013, 16. April & 23. May below) has sickened 113 people, 5 of whom are under 18, according to an update from the Centers for Disease Control and Prevention (CDC). The 113 confirmed cases are in the following 7 states: Arizona (15), California (57), Colorado (23), Hawaii (5), New Mexico (5), Nevada (5), and Utah (3). 50 people have been hospitalized. The case patients range in age from 2 to 84, although most are between the ages of 40 and 64. . (![]() Reference)
Reference)
A pit bull that attacked 4 children (aged 2, 6, 12 and 17 year) and an adult in central in the village of Arges near Toledo (Castile-La Mancha province) was infected with rabies, marking the 1st recorded case of the disease on the Iberian Peninsula in almost 4 decades. The dog was bred in Spain but spent 4 months in Morocco, only returning within the last month (sometime between 11. May 2013 and 10. June 2013). All victims received post exposure vaccination and the local authorities have ordered compulsory vaccination of all dogs and cats within 15 days and an 18 mile [~29 km] radius of where the attacks took place. Some 60.000 dogs in 56 villages are thought to be at risk. At least 7 dogs with an high level of suspicion for contact have been put in quarantine. Mainland Spain has officially been declared rabies free in 1975. There have been occasional examples recorded in Spain’s North African enclaves of Ceuta and Melilla, cities on Morocco’s Mediterranean coast. (![]() Reference)
Reference)
Chronological list of imported animal rabies to Europe and the US: ![]() Reference
Reference
Researchers have discovered a new virus in patients in Vietnam suffering from encephalitis. The virus was detected in 28 of 644 patients who had severe brain infections and in none of 122 patients who had non-infectious brain disorders, according to researchers at the Oxford University Clinical Research Unit, Wellcome Trust South East Asia Major Overseas Programme and the Academic Medical Center, University of Amsterdam. The new virus is tentatively called CyCV-VN and is part of a group of viruses known as Circoviridae known to circulate in animals such as birds and pigs. (![]() Reference)
Reference)
As of 19. June 2013, more than 26.000 cases of rubella have been reported in Poland since the beginning of 2013. The entire country is affected, but the western region (Malopolskie and Wielkopolskie provinces) has the highest number of cases. Other provinces with high numbers of cases include Lublin, Lubusz, Kuyavian-Pomeranian, Podkarpackie, Pomeranian, and Zachodniopomorskie (West Pomeranian). (![]() Reference)
Reference)
The Japanese National Institute of Infectious Diseases reported that as of 9. June 2013, there were 10.102 cases of rubella in Japan, 4 times more than last year’s 2392 cases. 5000 cases were recorded in the 1st 4 months of 2013. That implies that the past 2 months have doubled the number of cases. The latest week’s cases were highest in Osaka and Tokyo Prefectures with 129 and 82 new cases, respectively. The epidemic has been most prevalent among men from 20 to 40 years old, amounting for 75% of cases. (![]() Reference)
Reference)
The Ministry of Health in Saudi Arabia has announced Three additional laboratory-confirmed cases with Middle East respiratory syndrome coronavirus (MERS-CoV). The first patient is a 42-year-old man with an underlying medical condition from the Eastern region, the second patient is a 63-year-old woman with underlying medical conditions from Riyadh region and the third patient is a two-year-old child with an underlying medical condition from Jeddah. Additionally, four previously laboratory-confirmed cases have died.
Background: Globally, from September 2012 to date, WHO has been informed of a total of 64 laboratory-confirmed cases of infection with MERS-CoV, including 38 deaths. WHO has received reports of laboratory-confirmed cases originating in the following countries in the Middle East to date: Jordan, Qatar, Saudi Arabia, and the United Arab Emirates (UAE). France, Germany, Italy, Tunisia and the United Kingdom also reported laboratory-confirmed cases; they were either transferred there for care of the disease or returned from the Middle East and subsequently became ill. In France, Italy, Tunisia and the United Kingdom, there has been limited local transmission among patients who had not been to the Middle East but had been in close contact with the laboratory-confirmed or probable cases. (![]() Reference)
Reference)
The 1st confirmed case of the wild poliovirus (WPV1) in Somalia since 2007 has been reported in Mogadishu on 9. May 2013. Since then, 14 WPV cases have been reported and also 2 WPV cases in Kenya [see comment following this newswire as the total number of cases reported in Somalia and Kenya combined is 14. Experts have warned the outbreak could spread to neighbouring countries and a surveillance alert for polio has been issued to all countries across the Horn of Africa. There is a great risk that the disease can reach Somaliland. Globally, 3 countries remain polio endemic (Nigeria, Pakistan, and Afghanistan). As long as polio exists anywhere in the world, all children are at risk from polio if not vaccinated. (![]() Reference)
Reference)
Note on the detection of poliovirus in Israel: Traces of poliovirus have recently been detected in the sewage systems of a number of locations in Southern Israel, including Kiryat Gat and Ashdod. This follows the discovery of poliovirus in the Be’er Sheva sewage system 3. June 2013. (A similar polio virus strain has alos recently been found in Egypt). The Health Ministry believes that all of the traces of poliovirus originate in the Bedouin town of Rahat, after the virus was found in the sewers there at the end of March. The ministry has not received any reports of individuals contracting polio as a result, but is continuing to pursue its polio vaccination campaign among children and adults in the Negev town of Rahat, in an effort to head off an outbreak. The presence of poliovirus in Rahat’s sewage system is evidence that one or more residents of the town have been excreting the virus at its infectious stage. (![]() Reference)
Reference)
An 28 year old immigrant from Guatemala died while in US custody from rabieS in Corpus Christi [Texas], according to a statement from US Immigration and Customs Enforcement (ICE). The US Border Patrol apprehended the patient on 9 May 2013 after he entered the country illegally near Hidalgo [Texas]. On 18 May 2013, he was hospitalized after showing rabies-like symptoms. (![]() Reference)
Reference)
From 1. January to 12. May 2013 (epidemiologic week 19), 9249 suspected cases of meningitis, including 857 deaths (case fatality rate 9.3%), have been reported from 18 of the 19 African countries under enhanced surveillance for meningitis. The number of cases reported so far are the lowest recorded during the epidemic season in the last ten years. The decrease in the number of cases of meningitis reported during the period under review is thought to be due to the progressive introduction of the newly developed Meningococcal A conjugate vaccine in countries of the African Meningitis Belt since 2010. The introduction of this first meningococcal vaccine available for preventive purposes in Africa has enabled the immunization of over 100 million people from 10 countries in the `Meningitis Belt´ in the past three years (2010-2012). (![]() Reference) (Note: have a look under the link `Meningococcal meningitis surveillance Africa – WHO surveillance bulletins´ on the right panel of this website)
Reference) (Note: have a look under the link `Meningococcal meningitis surveillance Africa – WHO surveillance bulletins´ on the right panel of this website)
The Ministry of Health in Italy has notified the WHO of a laboratory-confirmed case with Middle East respiratory syndrome coronavirus (MERS-CoV) in a resident in the country. The patient is a 45-year-old man who recently travelled to Jordan. He returned to Italy on 25. May 2013 with symptoms of cough and fatigue. His condition deteriorated and he was hospitalized on 28. May and currently in a stable condition. A laboratory test confirmed MERS-CoV infection. Globally, since September 2012, the WHO reported a total of 51 laboratory-confirmed cases of MERS-CoV infection, including 30 deaths: 9 of these cases have been reported from countries in the WHO European Region and include 4 deaths (see postings from 8., 12. & 14. May below). (![]() Reference)
Reference)
Moroccan Health Defense Network revealed the 1st MERS-CoV case in Morocco involving a United Arab Emirates citizen who is a tourist. He was hospitalized in Sheikh Zayed’s hospital in Rabat on 29. May 2013. This is the 1st case reported from Morocco. Up to now most MERV-CoV infections have been recorded in Saudi Arabia. In addition cases have been reported from Jordan, Qatar, UK, UAE, Germany, Tunisia, and France. (![]() Reference)
Reference)
The Ministry of Health of Ethiopia is launching an emergency mass-vaccination campaign against yellow in response to six laboratory confirmed cases on 7 May 2013. The six laboratory-confirmed cases are from South Omo, in the Southern Nations, Nationalities and Peoples’ region. The cases were identified through the national surveillance programme for yellow fever. The index case was a 39-year-old man who presented with fever and jaundice and haemorrhagic signs in January 2013. (![]() Reference)
Reference)
Recently outbreaks of hepatitis A associated with consumption of meals prepared with frozen berries have been reported from British Columbia, five mainland US states, several countries in Northern Europe, and Italy (see posting from 16. April 2013 & 23. May below), and now Hawaii. Hawaii is the sixth US state to be added to the growing number of states reporting cases of hepatitis A outbreak. State health officials in Hawaii reported two cases, one from the island of Oahuand and the other from Kauai. In all cases the outbreak strain was identified as hepatitis A virus, genotype 1B, a genotype rarely seen in the Americas, but commoner in the Middle East. In the previous incidents the source of the berries was not determined, but in the most recent incident in Hawaii the origin of the frozen berries was reported to be from multiple locations (Argentina, Chile, and Turkey). The outbreaks in the United States appear to have been traced to a single supplier, but as yet there has been no recall of the product. Like at least another 30 victims on the mainland, the Hawaii residents are believed to have consumed a frozen organic berry mix purchased at local Costco outlets. (![]() Reference)
Reference)
The Venezuelan Health authorities have recorded 15 fatal cases of H1N1-Influenza in Zulia state (bordering Columbia). The cases were all male above 40 years. Currently a number of patients infected with H1N1 influenca are hospitalized in Zulia state: Maracaibo (11), Lagunillas (3), Cabimas (3), San Francisco (2), Colón (2) und Sucre (1). (![]() Reference)
Reference)
Zika virus (ZIKV) has been detected in the blood of a 45 year old Canadian woman who recently returned from a vacation in southern Thailand (Phuket Island). ZIKV is a flavivirus which was first reported from Thailand in 1954. Three days after the patient return to Canada she developed fever, headache, chills, nausea (with vomiting), extreme fatigue, and noted blisters in her mouth. After a brief respite from her symptoms she developed severe backache with a papular rash, involving her extremities including her palms, for which she sought medical assistance at a local emergency department. Initial investigations included hemoglobulin (131 g/L), white blood cell count (4.7 x 109 /L), with a normal differential blood count, but with a low platelet count of 81 x 109 /L (normal range 150-400 x 109 /L). Creatinine, electrolytes, ALAT, and AP were normal. Thick and thin blood smears were negative for malaria. Blood cultures were negative for bacterial pathogens as was the measles RT-PCR performed on her nasopharyngeal swab and urine. A number of serum samples collected over 30 days were tested for dengue IgM and IgG antibodies. A sample collected on 15 Feb [2013], was negative, whereas a follow-up sample collected 4 days after the 1st specimen gave a positive result in the dengue IgM antibody EIA, although the IgG antibody was negative, consistent with an acute dengue fever infection. However, the lack of a dengue IgG seroconversion on a convalescent serum and the unusual nature of the rash, prompted further investigatations. Reverse-transcriptase PCR identified ZIKV. Subsequent serological testing of convalescent sera by the Centers for Disease Control, confirmed the presence of ZIKV specific neutralizing antibodies by a plaque reduction neutralization assay. The reactivity of the serum in the dengue IgM EIA is consistent with previously observed serological cross reactions involving the flaviviruses. The patient made a relatively uneventful recovery, about two and a half to three weeks after her initial symptoms. Background:![]() Zika virus (
Zika virus (![]() Reference)
Reference)
A chikungunya outbreak appears to have taken hold of Singapore, with over 60 reported cases this month alone [May 2013]. This brings this year’s total to 184, more than 3 times the 60 annual cases that were reported over the past 3 years. A Ministry of Health spokesman said at least 37 of those identified with the disease are locals and 2 were hospitalised but have been discharged. (![]() Reference)
Reference)
As of 20. May 2013, 7 laboratory confirmed cases of Crimean-Congo hemorrhagic fever (CCHF) have been reported in the Rostov Region: 4 cases were recorded in the Salsk district region, 2 in the Proletarsk district, and 1 in the Martynovsky district. The situation with regard to CCHF in the Rostov region is worrying. The majority of municipalities lie in territory that includes natural foci of CCHF infection. According to recent data last month [April 2013] 403 persons, including 124 children under 14 years old, sought treatment for tick bites. The largest number of such cases were registered in the Rostov-on-Don, Volgodonsk, Taganrog, Salsk, Peschanokopsk, Semikarakorsk, Tselinsky and Salsk areas. The natural tick foci responsible for CCHF infection include steppe, semi-desert, and forest-steppe landscapes of the south of Russia: including Kalmykia, Dagestan, Ingushetia, Karachaevo-Cherkessia and Kabardino-Balkaria, Krasnodar, Stavropol , Rostov, Volgograd, and Astrakhan regions. (![]() Reference) (Background on CCHF: see posting from 15. Janary 2013 below)
Reference) (Background on CCHF: see posting from 15. Janary 2013 below)
In April 2013, ten cases of dengue fever in residents and travelers returning from Luanda, Angola, to five countries on four continents, were reported to the GeoSentinel Surveillance network. Dengue virus serotype 1 was identified in two cases. (![]() Reference)
Reference)
An increase in dengue fever in returning travelers from Angola was reported from our TropNet centre in Lisbon, Portugal on 14. May 2013: Eight patients were diagnosed in March 2013, 7 of then in the last two weeks of this month; eleven additional patients were diagnosed in April. Patients were residents or travelers to the Luanda metropolitan area, Angola and most of then were Portuguese. Dengue virus serotype 1 DENV1 was confirmed in 4 cases.
Bosnia and Herzegovina:
From August 2012 – April 2013, an outbreak of hepatitis A with 28 laboratory-confirmed cases occurred in Bijeljina, Bosnia & Herzegovina. The index case was in a 7-year-old child from the local Roma [gypsy] community. (![]() Reference)
Reference)
Italy:
Travelers from various European countries have been infected with hepatitis A (subgenotype 1A) during traveling to North-East Italy between September 2012 and Mai 2013. Most cases have been reported during January – April 2013 (ski holidays). Among Italians the increase in cases of hepatitis A (417 cases since September 2012) was significantly raised compared to same period last year (167 cases). Frozen berries are suspected to be the source of infection (similar to the outbreak reported from Northern Europe between October 2012 and April 2013; see posting from 16. April 2013 below). (![]() Reference)
Reference)
The case of a 20-year-old woman from Papua New Guinea (PNG) who had been hospitalized in Queensland in an isolation ward since May 2012 and who died on 14. March 2013 in Cairns Base Hospital with XDR-TB (extensively drug resistant TB) has been reported. She was said to be part of an ongoing TB epidemic in PNG on Daru Island, capital of PNG’s Western Province that is located just north of the Torres Strait and Cape York Peninsula (Far North Queensland) at the tip of the state of Queensland, Australia. Currently approximately 60 contacts (persons who had more than 8 hours contact to the patient) are traced for screening. (![]() Reference,
Reference, ![]() Reference)
Reference)
In the face of an update of the 2003 WHO position paper on the use of Yellow fever (YF) vaccines, the WHO strategic advisory group of experts on immunization (SAGE) reviewed the evidence of the current YF vaccination policy (in particular on the need for booster doses of YF vaccine every 10 years after primary vaccination and on the risk of serious adverse effects following immunization in the elderly). Based on currently available surveillance data, SAGE concluded that vaccine failures are extremely rare and do not cluster as time increases after immunization. Since yellow fever vaccination began in the 1930s, only 12 known cases of yellow fever post-vaccination have been identified, after 600 million doses have been dispensed. Evidence showed that among this small number of `vaccine failures´, all cases developed the disease within five years of vaccination. This demonstrates that immunity does not decrease with time. Therefore a single dose of YF vaccine is sufficient to confer sustained immunity and life-long protection against YF and a booster dose of YF vaccine is not needed. (Surveillance in endemic countries and future clinical studies may possibly identify specific risk groups (such as infants or HIV-infected patients) that could benefit from a second primary or booster dose). SAGE requested WHO to revisit the international health regulation (IHR) provisions relating to the period of validity for international certificates for vaccination against YF. (![]()
![]() Reference)
Reference)
What changes for travelers ?
- Because the health authorities of all YF endemic countries will have to first ratify the new WHO recommendations, all travellers requiring YF vaccination proof at immigration/transit (according to the international health regulations) will still need to be vaccinated within the last 10 years. Therefore the obligatory YF vaccination regulations remain unchanged.
- For travelers visiting YF endemic countries where YF vaccination is recommended but not obligatory a booster dose of YF vaccine is not longer recommended if the traveler had been vaccinated in the past. (Exceptions for immunocompromised patients etc. remain unchanged).
- An expiry date of the YF immunisation protection is not longer recorded in the vaccination passport. Solely the date of the validity of YF protection is recorded.
The Tunesian Ministry of Health announced the death of a Tunisian citizen returning from the Gulf with an infection by the novel coronavirus (MERS-CoV = `Middle East Respiratory Syndrome Coronavirus´). The patient was a 66 years old diabetic patient, who was treated in the Fatima Bourguiba Hospital in Monastir for acute respiratory insufficiency upon his return from a trip to Saudi Arabia and Qatar where one of his sons lives. Medical evaluation of his family revealed 2 of his sons had symptoms [consistent with an influenza-like illness] but completely recovered [the translation here is not clear whether their infection was laboratory confirmed]. This case represents the 1st reported case of MERS-CoV in a returning traveler from Tunisia. (![]() Reference)
Reference)
51 people living in Rio Segundo, Cordoba, Pilar and Laguna Larga have been diagnosed with trichinellosis. The source of infection is salami made from home slaughtered meat without veterinary inspection. So far 51 cases have been confirmed, affecting people of Rio Segundo (21), the city of Cordoba (13), Pilar (13) and Laguna Larga (4). Although no serious/life-threatening cases have been observed, 2 people required hospitalization in Rio Segundo. Sausages consumed by the infected people were in all cases acquired in licensed shops, including supermarkets, butchers and other stores. (![]() Reference)
Reference)
An outbreak of dengue in Mombasa, Kenya, has been reported by the Kenyan Ministry of Public Health and Sanitation (MOPHS). Mombasa is the second-largest city in Kenya and is a major shipping port and tourist destination. This is the first identified dengue outbreak in Mombasa since 1982. (![]() Reference)
Reference)
Cutaneous leishmaniasis is on the rise in Pakistan’s Federally Administered Tribal Areas (FATA), according to reports by FATA’s Directorate of Health. The recent surge in cases saw 1335 patients with cutaneous leishmaniasis treated from January to March 2013, according to the FATA Directorate of Health, an increase of over 270 cases compared to the same period last year [2012]. MSF donated 1200 vials of the drug Meglumine Antimoniate (Glucantime) in the last week of April [2013]. This was almost 30 percent of the quantity that had been requested across FATA for an entire year, based on last year’s patient numbers. Since the 1st reported outbreak in FATA in 2002, the Health Directorate launched a national response programme in 2003 to tackle the disease. During 2012, MSF treated 298 patients for the disease at the Sadda Tehsil Headquarter hospital in Kurram Agency. (![]() Reference)
Reference)
A Filipino migrant worker is the 1st case of human rabies to be reported from Taiwan in 2013, according to the Taiwnese Centers for Disease Contol (CDC): A 31-year-old Filipino man apparently received a dog bite on 10. March 2013 and failed to receive post-exposure vaccination. He arrived in Taiwan in early April 2013 and started to experience early symptoms of rabies last week [week of 6 May 2013]. At admission the physician at the hospital noticed the healing dog bite on the patients fingers and the family confirmed the animal bite. The patient’s condition is deteriorating rapidly and he is now suffering from multiple organ failure. (![]() Reference)
Reference)
Saudi Arabia has confirmed 4 new cases of the SARS-like coronavirus in its Eastern Province. The health ministry reported that one of the 4 new cases has already been released from the hospital, while the 3 other new cases are still hospitalized [13 May 2013]. (![]() Reference)
Reference)
Background: As of May 2013, a total of 40 people in Saudi Arabia, Qatar, Jordan, the United Kingdom (UK), the United Arab Emirates, and France were confirmed to have respiratory illness caused by a novel (new) coronavirus. Twenty of these 40 people died. In the UK, an infected man likely spread the virus to two family members. He had recently traveled to Pakistan and Saudi Arabia and got sick before returning to the UK. In Saudi Arabia, two health care providers were infected after caring for patients who had novel coronavirus. Clusters of cases in Saudi Arabia, Jordan, the UK, and France are under investigation.
The Ministry of Social Affairs and Health in France has informed WHO of an additional laboratory-confirmed case with infection of the novel coronavirus (NCoV). This patient was identified as part of the epidemiological investigation initiated by the French authorities, following laboratory confirmation of the first case on 7 May 2013. The patient shared a hospital room in Valenciennes with the first laboratory-confirmed patient from 27 to 29 April 2013. The patient is currently hospitalized and isolated in an infectious disease hospital. Among 120 persons identified as contacts of the first laboratory-confirmed case in France, laboratory tests were conducted by Pasteur Institute in Paris on five suspected cases, of which four tested negative, one (mentioned above) tested positive. In Saudi Arabia, an investigation is ongoing into an outbreak in a health care facility, where 15 patients, including seven deaths have been confirmed. From September 2012 to date, WHO has been informed of a global total of 34 laboratory confirmed cases of human infection with nCoV, including 18 deaths. (![]() Reference)
Reference)
The Ministry of Social Affairs and Health in France has informed WHO of one confirmed case with infection of the novel coronavirus (NCoV). The patient had an underlying medical condition, including an immunocompromised state. The patient became ill on 23 April 2013 and later developed respiratory symptoms. The nCoV infection was confirmed on 7 May 2013 by Institut Pasteur. The laboratory confirmation was obtained from a bronchoalveolar lavage specimen after a nasopharyngeal specimen tested negative. The patient is currently hospitalized. Preliminary investigation reveals that the patient had a history of travel to Dubai, United Arab Emirates. Further investigation into the case is ongoing. (![]() Reference)
Reference)
Background: (see posting from 6., 12., 26. March 2013 below) From September 2012 to date, WHO has been informed of a global total of 31 laboratory confirmed cases of human infection with nCoV, including 18 deaths. Based on the current situation and available information, WHO encourages all Member States (MS) to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. The newest case re-emphasizes the need for vigilance in recent travelers returning from areas affected by the virus and the need to use lower respiratory tract specimens for diagnosis when they can be obtained. WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions.
Since November 2012, there has been an increase in reported cases of hepatitis A in tourists returning from Egypt in several European countries (Denmark, England, Germany, The Netherlands, Norway, Sweden). As of 24 April, 80 HAV cases in travellers with symptom onset after 1. November 2012 visiting different areas in Egypt have been reported. Four cases from Norway, six cases from the Netherlands and five cases from England share an identical hepatitis A viral RNA sequence. This increase in cases suggests that vaccination recommendations for travellers to hepatitis A endemic countries should be reinforced. (![]() Reference)
Reference)
To date, a total number of 108 laboratory-confirmed cases of human infection with avian influenza A(H7N9) virus (including 22 deaths) have been reported from China. On 24. April one additional laboratory-confirmed case has been reported from Taiwan (the patient acquired the infection while working in China). Investigations into the possible sources of infection and reservoirs of the virus are ongoing. Until the source of infection has been identified, it is expected that there will be further cases of human infection with the virus. So far, there is no evidence of sustained human-to-human transmission. (![]() Reference)
Reference)
On 14. April the death of a 6-year-old boy due to Bolivian hemorrhagic fever (Machupo virus) has been reported from the town of Magdalena in Beni department. So far in 2013 there were 115 suspected/13 confirmed cases in the whole Beni department. In 2012 a total number of 13 confirmed human cases (including 7 fatal) had been reported from Beni department. Beni department (![]() map) has been a recognized as endemic region for Machupo virus infections (Bolivian hemorrhagic fever) since the virus was first isolated in Bolivia in 1959. (
map) has been a recognized as endemic region for Machupo virus infections (Bolivian hemorrhagic fever) since the virus was first isolated in Bolivia in 1959. (![]() Reference)
Reference)
As of 17. April 2013 a total of 82 patients (including 17 fatal cases) have been laboratory-confirmed with human infection with avian influenza A(H7N9) virus in China. More than a thousand close contacts of the confirmed cases are being closely monitored. Epidemiological investigations into the possible sources of infection and reservoirs of the virus are continuing (see posting from 12. April below). So far, there is no evidence of ongoing human-to-human transmission. The WHO does not advise special screening at points of entry with regard to this event, nor does it recommend that any travel or trade restrictions be applied. (![]() Reference)
Reference)
An outbreak of hepatitis A infection has been reported in Denmark, Finland, Norway and Sweden over the last six months with 66 cases as of 11. April 2013. Sixteen of the cases were due to genotype 1b with identical RNA sequence. None of the cases have travel history outside the EU within the period of their potential exposure. There are 50 additional non-travel related cases of hepatitis A reported in the four countries for whom the sequence is not known. Epidemiological investigations in Denmark, Finland and Sweden revealed that all the patients had consumed berries, in particular frozen berries in smoothies. Strawberries were the food item having the strongest association with the infection. No hepatitis A virus could be isolated from food samples so far. Food Safety Authorities and Public Health Authorities in the affected countries are currently collaborating to uncover the source of the infection. (![]()
![]() Reference)
Reference)
A 7-year-old girl is reported to be the 1st case diagnosed with H7N9 avian influenza in Beijing. The girl girl’s parents were reported to be engaged in live poultry trading in a township of Shunyi District in Beijing’s northeastern suburbs. This first case in Beijing raises the number of H7N9 infections in China to 44 (see posting below). (![]() Reference)
Reference)
As of 11. April 2012, a total of 38 patients have been laboratory confirmed with influenza A(H7N9) virus infection in China, including 10 deaths, 19 severe cases and 9 mild cases (![]() Reference). While the quest for the source of the outbreak is still continuing on multiple fronts it remains unclear, whether this novel avian influenza virus — first reported in humans in China less than two weeks ago — will rapidly fizzle out, become established in animal hosts to fuel future human outbreaks, or morph into a virus that can spread easily between people and spark a pandemic. So far, epidemiological investigations of the cases remain largely inconclusive: patients have been reported from 11 cities, some a few hundred kilometres apart; some patients had contact with poultry or other animals just before falling ill, whereas others had not; late last week, the H7N9 virus was found in chikens, pigeons and ducks at bird markets in Shanghai, Nanjing and Hangzhou. Although the virus might have come from other sources, including mammals, the pattern of many human cases over a wide area in a short time could be explained by live markets alone, because birds from one or a few sources might have been transported to multiple markets. But the various bird species found to be infected may not be the original source, because much cross-infection can occur in live markets. Researchers know that the virus mainly infects wild birds such as ducks, geese, waders, and gulls, and that they occasionally jump into poultry flocks. However, the H7N9 virus has not been detected in wild birds so far. Wherever the virus originated, a crucial question is whether it could become established in poultry, creating a reservoir that might lead to continued, sporadic human infections. Unlike its cousin H5N1 – which has killed millions of birds and several hundred people in Asia and elsewhere since 2003 – H7N9 does not cause serious bird disease, which might greatly complicate efforts to control it. It would be next to impossible to detect H7N9 through routine surveillance for sick poultry among China’s 6 billion domestic birds. As humanity has never been widely exposed to H7 or N9 flu viruses, resistance to these subtypes is lacking. This lack of acquired immunity would favour pandemic spread if human-to-human transmission evolves, which currently has not been observed. (
Reference). While the quest for the source of the outbreak is still continuing on multiple fronts it remains unclear, whether this novel avian influenza virus — first reported in humans in China less than two weeks ago — will rapidly fizzle out, become established in animal hosts to fuel future human outbreaks, or morph into a virus that can spread easily between people and spark a pandemic. So far, epidemiological investigations of the cases remain largely inconclusive: patients have been reported from 11 cities, some a few hundred kilometres apart; some patients had contact with poultry or other animals just before falling ill, whereas others had not; late last week, the H7N9 virus was found in chikens, pigeons and ducks at bird markets in Shanghai, Nanjing and Hangzhou. Although the virus might have come from other sources, including mammals, the pattern of many human cases over a wide area in a short time could be explained by live markets alone, because birds from one or a few sources might have been transported to multiple markets. But the various bird species found to be infected may not be the original source, because much cross-infection can occur in live markets. Researchers know that the virus mainly infects wild birds such as ducks, geese, waders, and gulls, and that they occasionally jump into poultry flocks. However, the H7N9 virus has not been detected in wild birds so far. Wherever the virus originated, a crucial question is whether it could become established in poultry, creating a reservoir that might lead to continued, sporadic human infections. Unlike its cousin H5N1 – which has killed millions of birds and several hundred people in Asia and elsewhere since 2003 – H7N9 does not cause serious bird disease, which might greatly complicate efforts to control it. It would be next to impossible to detect H7N9 through routine surveillance for sick poultry among China’s 6 billion domestic birds. As humanity has never been widely exposed to H7 or N9 flu viruses, resistance to these subtypes is lacking. This lack of acquired immunity would favour pandemic spread if human-to-human transmission evolves, which currently has not been observed. (![]() Reference)
Reference)
The UOSSM [Union of Syrian Medical Relief Organizations] called on the World Health organization and the international medical agencies to assist the local health care providers and public health centers inside Syria and on the Turkish border in treating the escalating number of leishmaniasis. It is estimatee that as many as 100.000 people have been infected in the past 2 years after civil war broke out in Syria, compared with before the conflict when the number of leishmania cases in Syria had been reduced to 3000-4000 per year. (![]() Reference)
Reference)
To date, a total of 24 cases of H7N9 avian influenza virus infection have been laboratory confirmed in China, including 7 deaths, 14 severe cases, and 3 mild cases. More than 600 close contacts of the confirmed cases are currently being monitored. In Jiangsu, investigation is ongoing into a contact of an earlier confirmed case who developed symptoms of illness. However, at this time there is no evidence of ongoing human-to-human transmission. No vaccine is currently available for this subtype of the influenza virus. Preliminary test results provided by the WHO Collaborating Centre in China suggest that the virus is susceptible to the neuraminidase inhibitors (oseltamivir and zanamivir). (![]() Reference)
Reference)
Just published in NATURE: ‘The global distribution and burden of dengue’ (![]() Reference): The authors undertook an exhaustive assembly of known records of dengue occurrence worldwide and used a formal modelling framework to map the global distribution of dengue risk. The authors then paired the resulting risk maps with detailed longitudinal information from dengue cohort studies and population surfaces. The authors estimate the total worldwide burden of dengue to be as high as 390 million infections per year, which is more than three times the dengue burden estimate of the World Health Organization.
Reference): The authors undertook an exhaustive assembly of known records of dengue occurrence worldwide and used a formal modelling framework to map the global distribution of dengue risk. The authors then paired the resulting risk maps with detailed longitudinal information from dengue cohort studies and population surfaces. The authors estimate the total worldwide burden of dengue to be as high as 390 million infections per year, which is more than three times the dengue burden estimate of the World Health Organization.
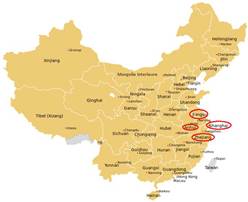
Since the posting from 1. April (see below) 2 additional fatal cases of H7N9 infection have been reported: On 3. April the 3rd fatal case of H7N9 infection (a 38-year-old man from Zhejiang province (close to Shanghai)) has been reported (![]() Reference). On 4. April the 4th fatal case of H7N9 infection (a 48-year-old man from Jiangsu who died in Shanghai) has been reported (
Reference). On 4. April the 4th fatal case of H7N9 infection (a 48-year-old man from Jiangsu who died in Shanghai) has been reported (![]() Reference). With these 2 additional cases the death toll has risen to 4. The number of human infections currently reported is at 11:
Reference). With these 2 additional cases the death toll has risen to 4. The number of human infections currently reported is at 11:
1. Shanghai Male 87 y. Died on 4. March 2013
2. Shanghai Male 27 y. Died on 10. March 2013
3. Anhui Female 35 y. Symptoms onset 15/03. Hospitalized in Jiangsu. Severe condition.
4. Jiangsu Female 45 y. Symptoms onset 19. February 2013. Critical condition.
5. Jiangsu Female 48 y. Symptoms onset 19. February 2013. Critical condition.
6. Jiangsu Male 83 y. Symptoms onset 20. February 2013. Critical condition.
7. Jiangsu Female 32 y. Symptoms onset 21. February 2013. Critical condition.
8. Zhejiang Male 38 y. Symptoms onset 7. March 2013. Died on 27. March 2013.
9. Zhejiang Male 67 y. From Hangzhou. Hospitalised 25 March 2013.
10.Zhejiang Male 64 y. Symptoms onset 29 March, Hospitalised 31 March 2013.
11.Jiangsu Male 48 y. Died on 4. April 2013.
(EpiSouth Weekly Bulletin No. 263)
So far, 2 men suffering from a lesser-known type of bird flu have died in Shanghai and a woman in eastern Anhui Province is in a critical condition. The 3 cases of H7N9 avian influenza infection are the 1st time the virus has been detected in humans. The men were a 87-year-old who became ill on 19. Feb. 2013 and died on 4. Mar. 2013, and a 27-year-old who became ill on 27. Feb. 2013 and died on 10. Mar. 2013. A 35-year-old woman from Chuzhou City in Anhui became ill on 9. Mar. 2013 and is being treated in Nanjing, capital of Jiangsu Province. All 3 showed initial symptoms of fever and coughing which developed into severe pneumonia with difficulty in breathing in later stages, according to the commission. There was no sign that any of the 3 had contracted the disease from each other, and no sign of infection in the 88 people who had closest contact with them. H7N9 avian influenza virus is considered a low pathogenic strain that cannot easily be contracted by humans. The overwhelming majority of human deaths from bird flu has been caused by the more virulent H5N1 virus, which decimated poultry stocks across Asia [beginning] in 2003. To date there is no evidence of human-to-human transmission of H7N9 and therefore the risk to public health is currently considered low. It is still unclear how the 3 patient got infected. China’s CDC suspects that the source of the infections is probably poultry as H7 influenza infections in humans are uncommon but have been confirmed in people who have direct contact with infected birds, especially during H7 outbreaks. Between 1996 and 2009, human H7 infections were reported in the Netherlands, Italy, Canada, the United States, and England, with pathogens including H7N2, H7N3, and H7N7. Most of the infections involved conjunctivitis and mild upper respiratory symptoms. (![]() Xinhuanet;
Xinhuanet; ![]() WHO)
WHO)
Coccidioidomycosis (`Valley fever´), a fungal infection appears to be on the rise in the southwestern U.S. According to CDC data the number of cases
has increased nearly 10-fold between 1998 and 2011: cases in Arizona, California, Nevada, New Mexico and Utah rose from 2265 in 1998 to more than 22.000 in 2011. The CDC found that between 1998 and 2011 cases of valley fever went up 16% per year in Arizona and 13% per year in California (with more than 90% of cases reported by these 2 states). (![]() Reference)
Reference)
Background: Coccidioidomycosis (commonly known as “Valley fever”, “California fever”, “Desert rheumatism”, or “San Joaquin Valley fever”) is a fungal disease caused by Coccidioides immitis or C. posadasii. It is endemic in certain parts of Arizona, California, Nevada, New Mexico, Texas, Utah and northwestern Mexico. C. immitis resides in the soil in certain parts of the southwestern United States, northern Mexico, and parts of Central and South America. The spores, known as arthroconidia, are swept into the air by the wind and the frequent dust storms occuring in these regions. Infection is caused by inhalation of the particles. The disease mostly presents as an influenza-like illness with fever, cough, headaches, rash, myalgias, and arthralgias and is not transmitted from person to person. According to the CDC 30-60% of people who live in a region where the fungus is endemic will breathe it in at some point. An estimated 150.000 people are infected every year, but many don’t know they have anything other than a cold, and they get better on their own. The elderly and other people with weakened immune systems, such as HIV patients, are especially vulnerable. According to the University of Arizona, 60% of those infected don’t suffer any symptoms, and another 30% have just mild to moderate infections. 5 – 10% may suffer from complications, and 1% of victims die. In immunocompetent patients the infection ordinarily resolves spontaneously. Antimicrobial therapy is mostly reserved for severe cases (mostly for immunocompromised individuals, in whom the disease can manifest in a disseminated form).
In December 2008, the Indonesian Ministry of Agriculture reported a rabies outbreak in dogs on the island of Bali, Indonesia, to the World Organization for Animal Health after the 1st human cases were reported in Denpasar and Badung districts in November 2008.
Human rabies cases:
2008: 4
2009: 48
2010: 82
2011: 24
2012: 8
After a mass dog vaccination program was implemented in 2010, a reduction in cases started to be seen. According to agency records, the latest mass rabies vaccination program included 80% of the dog population on the island, around 250.000 dogs. Now almost a year has passed since the last human rabies case has been reported from Bali in April 2012. Since the outbreak started in 2008 rabies vaccination distribution has become more selective these days: The rabies vaccine is prioritized for multiple and deep wounds caused by stray dogs. Free-of-charge rabies inoculations are provided at state-owned hospitals only for dog bite wounds in vital organs, including the head, face, fingers and genitalia. The vaccine can also be purchased at medical clinics. Last week, the Bali Health Agency stocked up with 5000 vials of anti-rabies vaccine that is estimated to be sufficient for around 1250 people for the next few months. In addition stage 4 of the mass dog vaccination for all the 300.000 dogs in Bali will start in mid-April 2013 and run until June 2013. The Bali administration is confident that the island will be able to achieve its target of being free from rabies by 2015. To be acknowledged with the status “rabies free,” Bali has to have 2 consecutive years without a single occurrence of rabies in either animals or humans. (![]() Reference)
Reference)
On 25. March 2013, an outbreak of dengue was reported in the port of Mombasa in southern Kenya (with at least two cases confirmed by the Kenya Medical Research Institute). The serotype and the total number of confirmed / suspect cases are not yet known.
Background: Early January 2013, cases have been reported in the North of the country. In September 2011, outbreaks of DEN-3 were confirmed in several Northern cities in Kenya, including Mandera (bordering Somalia and Ethiopia) and Wajir, with at least 5,000 suspected cases. The occurrence of an outbreak of dengue fever in Kenya is not unexpected. Given the lack of a monitoring system dedicated to arboviruses in Kenya and other African countries, very few outbreaks are identified and reported. In this area, peak of transmission often occurs after the rainy season. In the Indian Ocean, probable and suspect cases of dengue (DENV-1 serotype) have been reported from the Seychelles (74 cases from late January 2013 to 8. March 2013) and in the Reunion island (6 cases since 15. March 2013). Depending on the dynamics of the epidemic in Kenya, potential spreading to East Africa and Indian Ocean is not unexpected. (EpiSouth Weekly Bulletin No. 262)
The Robert Koch Institute informed the WHO of a new confirmed case of infection with the novel coronavirus (nCoV). The patient was a 73-year-old male from United Arab Emirates, who was transferred from a hospital in Abu Dhabi to Munich by air ambulance on 19 March 2013. He died on 26 March 2013.
In the United Kingdom, the index patient in the family cluster reported on 11 February 2013 (see posting from 12th Feb. 2013 below) with travel history to Pakistan and Saudi Arabia prior to his illness, has died. To date, WHO has been informed of a global total of 17 confirmed cases of human infection with nCoV, including 11 deaths. (![]() Reference)
Reference)
Summary of cases: 17 confirmed cases (11 deaths):
– Saudi Arabia: 9 cases (6 deaths)
– Jordan: 2 cases (2 deaths)
– UK: 4 cases (2 deaths)
– Germany: 2 cases (1 death)
Scientists from King’s College London are warning that millions of people may be exposed to risk of developing kidney failure and bladder cancer by taking herbal medicines that are widely available in Asia. The medicines, used for a wide range of conditions including slimming, asthma, and arthritis, are derived from a botanical compound containing aristolochic acids. These products are now banned in the USA and many European countries but the herbs containing this toxic acid can still be bought in China and other countries in Asia and are also available worldwide over the internet. The scientists reviewed worldwide cases of aristolochic acid nephropathy (AAN), describe the pathophysiology, and propose strategies to help doctors identifying and treating patients more effectively. [Reference: Goekmen MR, Cosyns JP, Arlt VM, et al: The epidemiology, diagnosis and management of aristolochic acid nephropathy: a narrative review. Ann Intern Med. 19 Mar 2013; 158(6): 469-77] (![]() Reference)
Reference)
On 1. March 2013 the Greek Ministry of Rural Development and Food reported a rabid domestic cat in Trikala prefecture, Thessaly region. As of today, a total of 17 animal rabies cases were reported in Greece (Central Macedonia, Western Macedonia, and Thessaly) since the first report on disease reoccurrence on 19. October 2012 (See posting from 23. Oct. 2012 below). Until now, most cases occurred in foxes and in few dogs and were located in Central and Western Macedonia regions, at the border with Former Yugoslav Republic of Macedonia and Albania. The rabid cat was reported in Thessaly region which is located in the centre of Greece. Until these recent cases Greece was considered a rabies-free country since 1987. (EpiSouth Weekly Bulletin No. 261)
In late February [2013] a man died of rabies in Maryland nearly 18 months after he got a kidney from a donor in Pensacola, Florida. Doctors in Florida didn’t test the 20 year old donor for rabies before he died in September 2011. His heart, liver, and other kidney went to recipients in Florida, Georgia, and Illinois. Public health agencies in 5 states are currently assessing the rabies risk for hundreds of people who may have had close contact with the rabies infected organ donor and the 4 transplant recipients. The 3 asymptomatic organ recipients received rabies vaccination. The CDC is investigating how the transplant donor got infected with the raccoon rabies virus that has been found in his brain tissue and that of the Maryland patient. The donor was an outdoor enthusiast who might have been bitten by a wild animal in his native North Carolina before moving to Florida and beginning training as an Air Force aviation mechanic 17 weeks before his death. He had visited a clinic at the Pensacola Naval Air Station in August 2011 for abdominal pain and vomiting and was transferred to a civilian hospital 4 days later. The airman died of encephalitis of unknown origin (complicated by seizures) and severe gastroenteritis complicated by dehydration and electrolyte abnormalities. Why the patient was cleared for organ explantation remains unclear, as federal guidelines published last year [2012] for evaluating organ donors with encephalitis urge “extreme caution” if the suspected cause is possibly a viral pathogen, such as rabies. (![]() Reference)
Reference)
Transplant related rabies cases:
- 2004: laboratory confirmation of rabies as the cause of encephalitis in an organ donor and 3 organ recipients at Baylor University Medical Center in Dallas, Texas: link
- 2004: rabies in 3 of 6 patients who received organs from a donor who died in late December 2004: link
The Japanese Health, Labor and Welfare Ministry announced on Tuesday [12. March 2013] that it has retrospectively confirmed 3 more cases of the tickborne virus infection SFTS (Severe Fever with Thrombocytopenia Syndrome) in Japan between 2005 and 2012. In total 8 cases of SFTS have been recorded in Japan to date. At least 2 of the 8 cases had a fatal outcome, and one case had a record of tick bite. Besides China, where the disease and the virus were discovered in 2009, Japan is the only country where cases of SFTS have been recorded so far. (![]() Reference)
Reference)
Background: SFTS emerged in northeast and central China in 2009, where it was isolated from patients presenting with fever, vomiting, diarrhea, multiple organ failure, thrombocytopenia, leucopenia and elevated liver enzyme levels. The virus was identified as a novel phlebovirus (family Bunyaviridae) believed to be transmitted by ticks. SFTS has a fatality rate of 12% and as high as 30% in some areas. The virus has been found in the Chinese provinces of Anhui, Henan, Hubei, Jiangsu, Liaoning and Shandong. SFTS occurs in rural areas, from March to November, and a majority of cases are found from April to July. (![]() Reference)
Reference)
The Ministry of Health in Saudi Arabia has informed WHO of a new confirmed case of infection with the novel coronavirus (nCoV):
The patient, a 39-year-old male, developed symptoms on 24 February 2013. He was hospitalized on 28 February 2013 and died on 2. March 2013.
Preliminary investigation indicated that the patient had no contact with previously reported cases of nCoV infection. (![]() Reference) (see posting from 6. Mar. 2013 below)
Reference) (see posting from 6. Mar. 2013 below)
Summary of cases: 15 confirmed cases (9 deaths):
– Saudi Arabia: 8 cases (6 deaths).
– Jordan: 2 cases (2 deaths).
– UK: 4 cases (1 patient from Qatar – under treatment, 3 patients from UK – one with history of travel to Saudi Arabia and Pakistan prior to illness; 1 under treatment, 1 recovered, 1 death).
– Germany: 1 case (patient from Qatar – discharged)
A security guard in Barangay Mabolo is the 1st casualty of rabies in Cebu City this year [2013]. The victim was bitten by his own pet dog already last year (!) and ignored the advice of neighbors to immediately seek medical help and receive post-exposure prophylaxis. (![]() Reference)
Reference)
An outbreak of muscular sarcocystis-like illness among travelers visiting Tioman Island, Malaysia has been evidenced since summer 2011. As of November 2012, GeoSentinel has been notified of 100 reported patients with suspected muscular sarcocystosis [![]() Reference]. Starting in summer 2011, 35 patients were identified by early 2012 and traveled there mostly during July and August 2011. The epidemic is currently ongoing, with a 2nd wave of 65 reported new diseased travelers returning since summer 2012.
Reference]. Starting in summer 2011, 35 patients were identified by early 2012 and traveled there mostly during July and August 2011. The epidemic is currently ongoing, with a 2nd wave of 65 reported new diseased travelers returning since summer 2012.
A cluster of 12 patients returning from Peninsular Malaysia since late August 2012 were seen and followed in Bordeaux, France. In the period of September-October 2012, 12 patients (7 male, 5 female; aged 11-46 years) were referred to the Division of tropical medicine, University Hospital Center, Bordeaux, France, with febrile myalgia, unexplained blood eosinophilia, elevated CPK levels, and negative trichinellosis serology. Cases spent their vacation from 26 Jul to 25 Aug 2012 on the east coast of peninsular Malaysia. All patients belonged to a tourist group from southwestern France. The group was composed of 4 families. Almost all patients presented high-grade fever, fatigue, headache, moderate-to-severe myalgia, and arthralgia. Three cases experienced febrile illness for more than 14 days. 2 patients had suffered from diarrhoea and extensive maculo-papular rash. A muscle biopsy from one patient revealed intense myositis, but no intramuscular cysts. Half of patients healed using usual analgic treatments. 6 patients were given empirically albendazole 400 mg twice a day for 7 days and oral prednisone (0.5 mg/kg/day) for 3 days tapered over 2 days. 6 weeks later, 4 patients have still not recovered and were experiencing prolonged asthenia and myalgia. The patients were effectively treated with additional prednisone 0.5 mg/kg/day for 5 days and decreasing dosage over 14 days. By February 2012, one patient relapsed with musculoskeletal complaints.
Since the beginning of this outbreak in Malaysia, human muscular sarcocystosis is seen as a possible emerging foodborne zoonosis. The source of infection, specific species, and life cycle are to be elucidated, and the definitive animal host to be identified. Herein, humans are thought to become accidental intermediate hosts for zoonotic species by ingesting fecally-contaminated food or water material. Strikingly, it should be stressed that cats and macaques are numerous in Tioman Island and neighboring places, and are good candidates as infected predator animals. Overall, international travelers should be aware of the risk of acquiring this infection through genuine food habits. (![]() Reference) (see also postings from 24. August and 22. October 2012 below)
Reference) (see also postings from 24. August and 22. October 2012 below)
The Ministry of Health in Saudi Arabia has informed WHO of a new confirmed case of infection with the novel coronavirus (NCoV). A 69-year-old male, was hospitalized on the 10th Feb 2013 and died on the 19th Feb 2013. Preliminary investigation indicated that the patient had no contact with previously reported cases of NCoV infection and did not have recent history of travel. To date, WHO has been informed of a global total of 14 confirmed cases of human infection with NCoV, including 8 deaths; giving a case fatality rate of 57 percent. Of the total number, 7 cases, including 5 deaths, have been reported from Saudi Arabia. WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. As the total number of confirmed cases to date is small (14), the observed CFR of 57% may be a reflection of non-confirmation of milder illness associated with infection with this nCoV.
Summary of cases:
– Saudi Arabia: 7 cases (5 deaths).
– Jordan: 2 cases (2 deaths).
– UK: 4 cases (1 patient from Qatar – under treatment, 3 patients from UK – one with history of travel to Saudi Arabia and Pakistan prior to illness; 1 under treatment, 1 recovered, 1 death).
– Germany: 1 case (patient from Qatar – discharged).(![]() Reference)
Reference)
A man coming from Nepal after a 3-month travel is in medical isolation in South Texas, and is the 1st person to cross and be held in detention while infected with one of the most severe types of drug-resistant tuberculosis known today. He has been traveling for 3 months through 13 countries from Nepal through South Asia, Brazil, Mexico, and finally into Texas. His TB is resistant to at least 8 of the 15 or so standard drugs, according to a U.S. government. His XDR strain has been seen only once before in the U.S., in another patient of Nepalese origin, according to the government description. The Nepalese patient was taken into custody by the U.S. Border Patrol in late November 2012 as he tried to cross the border illegally near McAllen, Texas. Given how far and wide the patient ventured, he took a flight of more than 8 hours to Brazil and also traveled by car, boat and on foot, his case was reported to the WHO as having potentially widespread public-health impact. The WHO’s Stop TB Department said it is working with the CDC to inform affected countries about people who may have been exposed to the man.
XDR-TB is a particularly dangerous form of the disease that is resistant not only to the 2 most potent TB drugs but also to a handful of 2nd-line drugs. It is rare in the U.S. where only 6 cases were reported in 2011, according to the CDC. But it is a growing threat in countries including India and South Africa, where it has been found all over the country. The risk to the world is that the disease will migrate outward from these hot spots. Treatment options for XDR-TB are limited and can themselves be toxic. Nepal is known for innovative health programs, including some to fight TB. But like many countries, it has struggled with drug-resistant forms. Nepal reported more than 35,000 TB cases in 2011, and 2.9 percent of new and 12 percent of previously-treated TB cases are multidrug-resistant, according to WHO data. (Reference)
The 3rd phase of the vaccination campaign against YF, that caused the death of 171 people across Darfur, will be launched on 5th Mar 2013. About 200,000 people in 3 localities (Jebel Moon, Kulbus and Sirba) are to be vaccinated in this phase. No new cases of YF have been reported in the state in the last 2 months. The federal health minister announced that 6 million people across Darfur have been vaccinated against YF since the campaign started last November 2012. Approximately 7.5 million people live in Darfur, according to the last census in 2010. WHO registered over 840 people infected with YF in Darfur. Epidemic affected 35 out of 64 localities in the region since September last year. Central Darfur had 51.5% of the registered cases of YF. It was followed by North Darfur (21%), West Darfur (17.4%) and South Darfur (9.5%). East Darfur was the least affected province.(![]() Reference)
Reference)
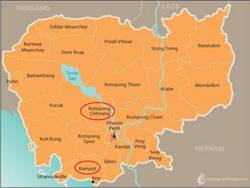
On 21 and 27 February 2013, the Cambodian Ministry of Health reported to WHO two new human cases of A(H5N1) influenza in Kampot and Kampong Cham provinces respectively. The case reported in Kampot province was a 20-month old boy with onset of symptoms on 6th Feb 2013, hospitalization on 18th Feb 2013, and who died on 19th Feb 2013. The case reported in Kampong Cham province was a 35-year old man with onset of symptoms on 8th Feb 2013, hospitalization on 13th Feb 2013, and who died on 25th Feb 2013. Both of them have been exposed to poultry. These two cases are the 8th and 9th case reported in Cambodia since the beginning of 2013. There is no epidemiological link between these two cases. Since 2003 a total of 30 cases have been confirmed in Cambodia, including 27 deaths.
A 53-year-old female traveller developed fever with headache, arthralgia, and exanthema in combination with lymphadenopathy and mild hepatitis 3 days after returning from an 18 day trip to Bali in December 2012. Laboratory diagnostics showed leucocytopenia, thrombocytopenia, and mildly elevated transaminases. Spite of negative serological results for chikungunya and dengue virus the PCR-result for chikungunya virus was positive. The virus strain could successfully be isolated by cell culture; molecular characterization of the isolated chikungunya virus is in progress. A second sample for serological follow up study 47 days after the 1st examination showed seroconversion for chikungunya virus with high titres for IgM- and IgG-antibodies. No serological evidence for a coinfection with dengue virus was found. The patient flighted directly from Germany to Bali. She predominantly stayed in the coastal region around Semenyak with excursions in the regions around Ubud. She reported several mosquito bites during her holidays but no clinical symptoms in Bali. Currently the patient still complains of headaches and arthralgia. While chikungunya fever cases in Indonesia seem to be frequent in Central and Western Java, there have been only sporadic reports from Bali so far. Travellers should be advised to apply preventive measures (such as, protection from mosquito bites) when visiting Bali.
Thailand: 7,033 people affected by dengue during the period between 1st Jan 2013 and 5th Feb 2013. Expected number of people around 100,000-120,000 people. Total deaths in 2013: 5 cases. The attack rate was 11.07 per 100,000 population. The case fatality rate (CFR) was 0.01 percent. The numbers of dengue cases have increased by a factor of 5.4, compared with the same period in 2012. The highest attack rate was reported in the south region (27.25), followed by the central region (11.62), the north region (7.61), and the northeastern region (5.78). The 5 provinces with the highest attack rates of dengue infection (per 100,000 population) were Songkhla (58.19), Krabi (56.03), Phatthalung (35.45), Surat Thani (34.20), and Rayong (34.15). The highest percentage of cases was reported in the 15-24 year old age group (27.14 percent), followed by the 10-14 year old age group (20.33 percent) and the 7-9 year old age group (11.55 percent).(![]()
![]() Reference)
Reference)
Asia
Philippines (Antique province): 33 cases; deaths 1.
Singapore: 232 cases in 2 urban areas; other areas 29 clusters.
Pacific
Australia (Cairns, northern Queensland state): since December 2012, 64 cases. Spreading. 2 separate outbreaks; dengue virus types 1, 3.
Africa:
Kenya (North Eastern province): An outbreak of dengue fever in northern Kenya (Mandera District), along the Ethiopian and Somali borders, is drawing attention to the need for improved health services in some of the country’s most remote communities. 3 suspected dengue deaths have been recorded, and there are fears that more cases have gone unreported. In 2011, an outbreak of dengue fever infected up to 5000 people.
Somalia (Mogadishu city): 28 cases.
Mexico: First 5 weeks of 2013, a total of 1061 cases; DHF/serious 355 cases; States most affected: Guerrero 209 cases, Veracruz 118 cases Michoacan 106 cases.
South America:
Argentina: 834 suspected cases, 22 confirmed cases.
Bolivia (Beni department): 2,537 suspected cases, 560 confirmed cases; 4 deaths; municipalities most affected are Guayaramerin with 235 confirmed cases, Riberalta with 209 cases, and Trinidad with 71 cases.
Brazil: Amazonas state with 726 cases; municipalities most affected are Manaus with 515 cases, Tabatinga with 125 cases, and Humaiata with 23 cases. Bauru, Sao Paulo state: 397 cases. Campinas, Sao Paulo state: 433 suspected cases, 84 confirmed cases; and DHF/serious 1 case. Belo Horizonte, Minas Gerais state: 1,097 suspected cases, 606 confirmed cases. Parana state: 3,150 confirmed cases; outbreaks in 11 municipalities. Rio de Janeiro state: 15,855 suspected cases; DHF/serious 8 cases. Sorocaba, Sao Paulo state: 132 cases; Deaths 1.
Colombia: 6,161 cases; DHF/serious 123 cases.Ecuador: 1,929 cases in 19 provinces; DHF/serious 19 cases; Deaths 4.
Paraguay: 23,917 suspected cases, and 14,518 confirmed cases.
Venezuela: 6,185 cases; DHF/serious 328 cases; States with outbreaks: Lara, Portuguesa, Barinas , Trujillo.
Following the emergence of 2 YF cases in the town of Goz Beida in Chad in December 2012, a 4-day vaccination campaign against the disease was launched on the 21st Feb 2013 in the close by Djabal camp for Sudanese refugees in the east of the country. The campaign target 17,375 residents. The vaccines are provided by Medecins Sans Frontieres. There are several Sudanese refugee camps in Chad due to the violence in the Darfur states. It is highly likely that there is a certain amount of movement across the Chad/Darfur porous border.(![]() Reference)
Reference)
Saudi Arabia: The Ministry of Health in Saudi Arabia has informed WHO of another confirmed case of NCoV infection. The patient was hospitalized on the 29th Jan 2013 and died on the 10th Feb 2013. The case was laboratory-confirmed on the 18th Feb 2013. Further investigation into this case is ongoing.
UK: Health Protection Agency continues to investigate the family cluster where 3 members of the family tested positive for NCoV infection. One member of this family, who had an underlying health condition, has died.
A total of 13 NCoV human cases have been confirmed by WHO, including 7 deaths.
WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. Testing for the NCoV should be considered in patients with unexplained pneumonias, or in patients with unexplained, severe, progressive or complicated respiratory illness not responding to treatment, particularly in persons traveling from or resident in areas of the world known to be affected.
Any clusters of SARI or SARI in healthcare workers should be thoroughly investigated, regardless of where in the world they occur.(![]() Reference)
Reference)
The Health Protection Agency continues its investigations into a family cluster of novel coronavirus infections in the UK. Three members of the same family have all tested positive for novel coronavirus. Two of these had no history of recent travel, suggesting that transmission has occurred in the UK. One person has died. This patient had an underlying condition that may have made them more susceptible to respiratory infections. The 1st patient in this cluster, who had recent travel history to Saudi Arabia and Pakistan, is still receiving treatment. The 3rd case, who had a mild illness, has recovered.
Since September 2012, when an earlier case was diagnosed in the UK, there have been a total of 12 confirmed cases of novel coronavirus reported globally, with 6 deaths. Intensive work has been carried out in the UK to identify contacts of the UK cases. In total, the HPA has identified and followed up on more than 100 people who had close contact with the cases in this recent family cluster. Besides the identified secondary cases, all tests carried out on contacts to date have been negative for the novel coronavirus infection.
The recent UK experience provides strong evidence of human-to-human transmission in at least some circumstances and it’s an important opportunity to obtain more information about the characteristics of this infection in humans and risk factors for its acquisition, particularly in the light of the 1st ever recorded instance of apparently lower severity of illness in one of the cases. The risk of infection in contacts in most circumstances is still considered to be low, and the risk associated with novel coronavirus to the general UK population remains very low. The HPA will continue to work closely with national and international health authorities and will share any further advice with health professionals and the public if and when more information becomes available.
Laboratory confirmed cases to date: 12 (6 deaths)
Saudi Arabia: 5 (3 deaths)
Jordan: 2 (2 deaths)
UK: 4 (1 patient from Qatar – receiving treatment, 3 patients from UK; 1 receiving treatment, 1 recovered, 1 death)
Germany: 1 (patient from Qatar – discharged)
(![]() Reference)
Reference)
The outbreak of Leishmaniasis that has affected the southern municipalities of Madrid in the last 3 years has not decreased in 2012, and 150 new cases have been reported last year. Nearly a total of 500 cases have been diagnosed since the beginning of the outbreak. The strong increase occurred from 2009, with 471 cases, compared to 15 or 25 that had been reported in previous years. All of the cases have been near the green area of Bosquesur, which officials believe may be the focus of leishmaniasis. This disease is transmitted by a sandfly that has previously bitten an infected animal. It is believed that hares and rabbits, which proliferate in Bosquesur, can act as reservoirs or carriers of the parasite. The outbreak is not considered to be over. So far this year 2013, there have been 3 new cases. Dogs are considered the main reservoir of Leishmania in Spain. It has been hypothesized that rabbits, hares, and squirrels may also be hosts, but this remains to be demonstrated.(![]() Reference)
Reference)
America- Dengue 2013:
Mexico- 1,061 cases; DHF 355 cases.
El Salvador- 377 cases.
Honduras (Olanch department). 50 cases, and increasing.
Dominican Republic- 1,323 cases; 3 Deaths.
Puerto Rico- 10,028 suspected cases, 467 confirmed cases; Dengue virus type 1 (79% of total cases), type 4 (21%), and increasing.
Bolivia- Cochabamba department: 9 confirmed cases, 126 suspected cases. Santa Cruz department: 40 confirmed cases; Deaths 1 (due to Dengue virus type 4 infection).
Brazil- Sorocaba, Sao Paulo state: 132 confirmed cases; Deaths 1, and increasing. Brazilia Federal District: 638 suspected cases, 160 confirmed cases. Goias: 20,793 reported cases. Goiania: 11,604 cases. Minas Gerais: 29,517 cases, 2 deaths. Parana: 3,439 cases.
Ecuador- 722 cases; 2 deaths. Paraguay- 34,612 suspected cases, 13,044 confirmed cases; 26 confirmed deaths and 12 suspected deaths; Dengue virus type 4 present. Venezuela- Carabobo state: 38 suspected cases; and increasing.
Asia- Dengue 2013:
Philippines (Misamis province)- 1,356 cases; 21 deaths. India (Mumbai, Maharashtra state)- 94 cases; and increasing. Pacific New Caledonia- Jan 2013: 965 cases, February 2013: nearly 500 cases; Deaths 1.
An hepatitis E outbreak has caused 111 deaths (total of diagnosed cases: 6,017) among refugees in camps of South Sudan since July 2012. The influx of people to the camps from neighbouring Sudan is believed to be one of the factors in the rapid spread of this viral disease. Hepatitis E virus is transmitted mainly through the faecal-oral route due to faecal contamination of drinking water. Other transmission routes include foodborne transmission from ingestion of products derived from infected animals and vertical transmission from a pregnant woman to her fetus. Currently, there is no vaccine available for control this virus infection. Hepatitis E virus infection is self-limiting in normal conditions, and fulminant hepatitis is rare, with only pregnant women being at increased risk. In environments such as the refugee camps in South Sudan, the outcomes are much more serious, especially for pregnant women.(![]() Reference)
Reference)
The Health Protection Agency confirm a 3rd case of novel coronavirus infection in a family cluster, following the 2 confirmed cases announced earlier this week. The patient, who is a UK resident and does not have any recent travel history, is recovering from a mild respiratory illness and is currently well. This latest case brings the total number of confirmed cases globally to 12, of which 4 have been diagnosed in the UK. Although this case appears to be due to person-to-person transmission, the risk of infection in contacts in most circumstances is still considered to be low. The risk associated with novel coronavirus to the general UK population remains very low.(![]() Reference)
Reference)
The dengue fever outbreak on Madeira (Portugal), which began in early October 2012, is still ongoing after January 2013, according to a ECDC Epidemiological Update of 14th Feb 2013. As of 3 Feb 2013, the Portuguese Ministry of Health has reported a total of 2,164 cases of dengue infection since 3rd Oct 2012. No deaths or cases of severe dengue have been reported. All reported cases refer to the resident population of the island. There have been 28 cases reported since the beginning of 2013. According to ECDC, 78 patients have been diagnosed in European countries with dengue infection after returning from Madeira: 11 in mainland Portugal, 23 in the UK, 19 in Germany, 3 in France, 5 in Sweden, 7 in Finland, 2 in Denmark, 2 in Austria, and 2 in Norway. Croatia, Slovenia, Spain and Switzerland have all reported one case each. The latest case was reported on the 1st Feb 2013 from Finland.(![]() Reference)
Reference)
A person from Oruro area, who had visited the tropics, died due to yellow fever in the Cochabamba department tropics. This occurrence put the health authorities on alert and they requested the populace to get vaccinated 10 days before traveling to the tropical area. Given the presence of the disease, it is recommended that before entering the topical area people must be vaccinated against yellow fever. YF virus is endemic in the Amazon Basin of the South American tropics. This is undoubtedly a case of jungle YF, where the virus infects wild primates and is transmitted to people by forest mosquitoes. It is critical that individuals in these areas be vaccinated against YF, to not only protect themselves, but to prevent introduction of the virus into the urban cycle where significant numbers of cases, with a high (30 per cent) case fatality may occur, as happened in Paraguay in 2008. It is good that the local health authorities have responded to the occurrence of this case.(![]() Reference)
Reference)
The Ethiopian government and the World Health Organisation have reported an outbreak of meningococcal meningitis around Arba Minch and Shebdino, in southern Ethiopia. There has been one reported case in Arba Minch town.(![]() Reference)
Reference)
The Ministry of Health of Chad is launching an emergency mass-vaccination campaign against yellow fever from 22 Feb 2013, following laboratory confirmation of 2 cases in the country in December 2012. The vaccination campaign will be conducted in 3 districts bordering Darfur, Sudan, namely Goz Beida, Guereda, and Adre, targeting over a million people, including inhabitants of refugee camps in the area. The campaign is supported by the Ministry of Health of Chad, the International Coordinating Group on Yellow Fever Vaccine Provision (YF-ICG11), and GAVI Alliance. These 2 cases were identified through the national surveillance programme for YF following intensive surveillance which was triggered in response to the YF outbreak in neighbouring Sudan’s Darfur region. The intensive surveillance in Chad also reported 139 suspected cases and 9 deaths. However, it is not clear whether these suspected cases were contracted in the same area of Chad, along the Darfur border, as the 2 fatal cases reported above. These cases are very likely spill-over from the YF outbreak in western or northern Darfur. The gold mines in Darfur had workers from other countries, most likely some from Chad, that might have contracted YF virus infections and returned home and died there.(![]() Reference)
Reference)
The Japan Health Ministry announced on the 13th Feb 2013 that 2 more people have been confirmed dead due to a viral infection transmitted by a mite bite. Total deaths caused by this virus infection are now 3. They died last fall 2012 from the infection, known as severe fever with thrombocytopenia syndrome (SFTS). They had no recent record of overseas travel. First case of SFTS was reported in China around 2009. Genetic studies showed the virus that killed the 3 Japanese occurred in Japan and did not come from China.
SFTS is a serious infectious disease with a 12 percent case-fatality rate that has been documented in 6 rural provinces in northeast and central China. SFTS is caused by a novel bunyavirus of the family Bunyaviridae, genus Phlebovirus. The major clinical signs and symptoms of SFTS are fever, thrombocytopenia, leukopenia, and elevated serum hepatic enzyme levels. The disease is believed to be transmitted by ticks because the virus has been detected in Haemaphysalis longicornis ticks. However, the disease can also be transmitted from person to person through contact with infected patients’ blood or mucous. SFTSV seroprevalence in the human population is unknown, and the natural reservoir hosts of SFTSV have not been determined.(![]() Reference)
Reference)
The UK Health Protection Agency confirm a further case of novel coronavirus infection in a family member of the case announced on 11 Feb 2013. The patient, who is a UK resident, does not have any recent travel history and is currently receiving intensive care treatment at The Queen Elizabeth Hospital, Birmingham. This patient has an existing medical condition that may make them more susceptible to respiratory infections. This latest case brings the total number of confirmed cases globally to 11, of which 3 have been diagnosed in the UK. Confirmed novel coronavirus infection in a person without travel history to the Middle East suggests that person-to-person transmission has occurred and that it occurred in the UK. Although this case provides strong evidence for person to person transmission, the risk of infection in most circumstances is still considered to be very low. If novel coronavirus were more infectious, a larger number of cases would have been diagnosed since the 1st case was reported 3 months ago. Therefore, the risk associated with novel coronavirus to the general UK population remains very low.
Laboratory confirmed cases to date: 11
Saudi Arabia: 5 (3 deaths)
Jordan: 2 (2 deaths)
UK: 3 (1 patient from Qatar – receiving treatment, 2 patients from UK, 1 with recent travel to Pakistan and Saudi Arabia – both receiving treatment)
Germany: 1 (patient from Qatar – discharged)
Coronaviruses are causes of the common cold but can also include more severe illness, such as SARS (severe acute respiratory syndrome). This new coronavirus was 1st identified in September 2012 in a patient who died from a severe respiratory infection in June 2012. The virus has so far only been identified in a small number of cases of acute, serious respiratory illness who presented with fever, cough, shortness of breath, and breathing difficulties.
(![]() Reference)
Reference)
Cambodia: a 4-year-old girl with avian influenza A/(H5N1) virus infection was reported on 13th Feb 2013, becoming the 7th person who was infected by the virus in 2013. This case is coming from Angkor Phnom Touch commune, Angkor Chey district of Southwestern Kampot province. 5 of 7 confirmed human H5N1 cases have been fatal in 2013. This is the worst outbreak of the virus since the disease was first identified in January 2004. To date, the country has recorded 28 human cases of the virus, 24 of them have had a fatal outcome. Of the 7 cases of avian A/(H5N1) virus infection confirmed in Cambodia in 2013, all have been children, and the majority female.(![]() Reference)
Reference)
China: One of 2 avian influenza A/(H5N1) infected people died of a multiple organ failure in a hospital in southwest China’s city of Guiyang on 13th Feb 2013. Epidemic control experts have not found any indication that the patients had close contact with birds, nor have they found any epidemiological connection between the two cases. People who have had close contact with the 2 patients have been put under medical observation. None have exhibited symptoms.
The Health Protection Agency (HPA) confirm the diagnosis of a further case of novel coronavirus infection in a UK resident, who had recently travelled to the Middle East and Pakistan. The patient is receiving intensive care treatment in a Manchester hospital. This latest case brings the total number of confirmed cases globally to 10, of which 2 have been diagnosed in the UK. Contacts of the case are also being followed up to check on their health. Risk associated with novel coronavirus to the general UK population remains extremely low and the risk to travellers to the Arabian Peninsula and surrounding countries remains very low. No travel restrictions are in place but people who develop severe respiratory symptoms, such as shortness of breath, within ten days of returning from these countries should seek medical advice and mention which countries they have visited. Coronaviruses are causes of the common cold but can also include more severe illness, such as SARS (Severe Acute Respiratory Syndrome). This new coronavirus was 1st identified in September 2012 in a patient who died from a severe respiratory infection in June 2012. The virus has so far only been identified in a small number of cases of acute, serious respiratory illness who presented with fever, cough, shortness of breath, and breathing difficulties.(![]() Reference)
Reference)
A 6 year old girl from Margao was diagnosed with rabies infection on 10th Feb 2013 at the Hospicio Hospital and is now undergoing treatment in an isolation ward. It appears that the patient had not received anti-rabies vaccine following a dog bite. The incident has caused a sense of alarm among the residents over the steep increase in the rise of the stray dog population in the city.(![]() Reference)
Reference)
The Federal and State Ministries of Health have started a vaccination campaign against yellow fever in Kabkabiya locality, North Darfur, in collaboration with the World Health Organization. The 3rd phase of the Darfur YF vaccination campaign was reported to have started on 26th Jan 2013 with coverage of more than 2 million people. There have been no newly reported suspected or confirmed YF cases since the 2 suspected cases were reported in West Darfur on 24th Jan 2013.(![]() Reference)
Reference)
Dengue fever among people between 15-35 years old in the southern region has increased in recent years, according to the Ho Chi Minh City Pasteur Institute. Last year 2012, the region registered 62,039 dengue fever cases, including children and adults, that is an increase of 11.2 per cent compared with 2011. Most of these cases were diagnosed in the south eastern region including 61 fatalities, with an increase of 3.4 per cent compared to 2011. The fatality rate rate and incidence among adults was 0.07 per cent and between fatality and serious incidence among adults, 2.06 per cent, which was 0.18 per cent higher than in 2011. Last year 2012, 511 patients had serious complications, including bleeding, kidney failure, and prolonged shock, and 11 of them died. Adults who are obese or have arthritis can develop more serious complications due to dengue fever.(![]() Reference)
Reference)
A New South Wales man has been confirmed as the 3rd fatality in Australia’s largest outbreak of listeriosis. A 68 year old man death occurred last January 2013 was confirmed by Victoria’s acting chief health officer as being linked to the outbreak at Jindi, one of the nation’s biggest cheese companies. A total of 26 cases have been identified so far, including a New South Wales woman who had a miscarriage. Victoria’s Department of Health maintains that it acted promptly to contain the outbreak. With an incubation period of up to 70 days, more cases of listeriosis associated with this outbreak can be expected.(![]() Reference)
Reference)
Two people in the city of Beijing died of rabies in January 2013. One of them was bitten by a stray dog on the finger; the other was bitten on the finger by a pet dog. None of them was vaccinated after the injuries. Most of the rabies cases in Beijing involve adult males who are farmers or migrant workers. Travellers to Beijing should be aware that canine rabies, despite rigorous control measures implemented by the local authorities, remains prevalent in the Chinese capital. Anyone injured in an encounter with a stray dog should seek immediate post-exposure prophylaxis. (![]() Reference)
Reference)
CDC of Taiwan revealed on the 31st Jan 2013 that a 48 year old man had been infected with Angiostrongylus cantonensis after eating undercooked snails. According to the CDC, the man had snail soup with 5 of his friends a few days before exhibiting symptoms of headaches and neck stiffness. The patient is still undergoing medical treatment in a hospital. His friends, who had snail soup with him, have not shown any symptoms of infection.
Humans are incidental hosts of this roundworm, and may become infected through ingestion of larvae in raw or undercooked snails or other vectors, or from contaminated water and vegetables. CDC said that people should wear gloves when handling snails and boil them for at least 3 minutes to avoid infection. A. cantonensis, also known as the rat lungworm, is prevalent in Southeast Asia and tropical Pacific islands. The recognized distribution of the parasite has been increasing over time and infections have been identified in other areas, including Africa, the Caribbean, and the United States. Small outbreaks and single cases of A. cantonensis are regularly seen in communities where consumption of raw snails is regarded as a delicacy. The infection may be overwhelming and lethal. Eosinophilia is the key finding which should lead to suspicion of A. cantonensis. (![]() Reference)
Reference)
The Ministry of Health (MoH) of the Kingdom of Cambodia reported 5 new human cases of avian influenza that were confirmed positive for the H5N1 virus in January 2013. Case details include 3 children and 2 adults from different areas of Cambodia. The cases all presented with fever, cough and other ILI symptoms. 4 of the cases died, with one case, the 8-month-old male, recovering after only experiencing mild ILI. Preliminary evidence does not support human-to-human transmission and 4 of the cases are known to have had close contact with sick/dead poultry. Results from testing of those who have ILI symptoms among close contacts for A/H5N1 influenza to date were negative. (![]() Reference)
Reference)
Outbreak of human Salmonella Typhimurium infections linked to contact with pet hedgehogs is historically rare, with only one to two cases reported via PulseNet annually since 2002. However, since 2011, an increasing number of cases have been detected. PulseNet identified 14 human isolates in 2011, 18 in 2012, and two in 2013. Since January 2012, a total of 20 persons infected with the outbreak strain of Salmonella Typhimurium have been reported from eight states. The median patient age was 13 years (range: <1–91 years); 55% of patients were female. Four patients were hospitalized. One death associated with Salmonella infection has been reported. Fourteen out of 15 patients (or their proxies) reported direct or indirect contact between the patient and a hedgehog during the week before illness onset. Children aged <5 years, elderly persons, and immunocompromised persons are at increased risk for severe illness. Infections can result from direct contact with hedgehogs during routine care and indirect transmission through contact with objects (e.g., cages, toys, or bedding) or household surfaces that come in contact with infected hedgehogs. (![]() Reference)
Reference)
Two more deaths caused by Nipah virus infection were reported on 27th of Jan 2013. Total deaths in 2013: 8. New deaths were from Pabna and Rajshahi.
The virus infects a person after drinking raw date sap and later on can be transmitted to other people through direct contact. It’s becoming a cause of public health concern in Bangladesh since 2001, as it breaks out every year during January-April. The Nipah virus fatality rate is nearly 80 per cent while it is fully preventable if people shun the consumption of raw date sap. Nipah virus was first detected in Malaysia in 1998 but at present Bangladesh, a hotspot for infectious diseases, is the only country in the world that reports the disease. (![]() Reference)
Reference)
An outbreak of Lassa fever in Lafia, the capital of Nasarawa State, was confirmed last week. Three cases with one fatality case have been reported. All of them were neighbours in Tudun Gwandara, an over-populated and one of the dirtiest sections of the metropolis.
Lassa fever is an acute viral illness that occurs in West Africa and it was named after the town in Nigeria where the first cases were originated. Lassa fever virus is a member of the virus family Arenaviridae, a single-stranded RNA virus, and is zoonotic. Lassa fever is mild or asymptomatic in about 80 percent of people but the remaining 20 percent have a severe multisystem disease. Lassa fever is also associated with occasional epidemics, during which the case-fatality rate can reach 50 percent. The reservoir, or host, of Lassa virus is a rodent known as the “multimammate rat” of the genus Mastomys. Lassa fever may also spread through person-to-person contact. The death rates are particularly high for women in the 3rd trimester of pregnancy, and for fetuses, about 95 percent of which die. Ribavirin has been used successfully in the treatment of Lassa fever patients (![]() Reference).
Reference).
An outbreak of cholera has been ongoing in Haiti since October 2010. According to the Ministere de la Sante Publique et de la Population (MSPP), as of December 31, 2012, 635,980 cases and 7,912 deaths have been reported since the cholera epidemic began in Haiti. Cases have been officially reported in all 10 departments of Haiti. In Port-au-Prince, the country’s capital, 173,485 cases have been reported since the beginning of the outbreak. Cases in Port-au-Prince have been reported from the following neighborhoods: Carrefour, Cite Soleil, Delmas, Kenscoff, Petion Ville, Port-au-Prince and Tabarre. (![]() Reference)
Reference)
Thailand (2012): 78,075 people were infected with dengue fever (81 of them fatally) last year 2012 and the spread of this disease will possibly be more serious this year 2013, according to the Public Health Ministry. Attack rate was 122 patients per 100,000 population with CFR of 0.10 percent. The highest number of 30,562 patients was reported in the central region, with Bangkok being the most affected area with 10,320 patients. In previous years, dengue fever mainly infected children but last year statistics found 52.44 per cent of patients were older than 15 years. (![]()
![]() Reference)
Reference)
Thailand (current year): from the beginning of 2013, a total of 971 cases and no deaths have been reported. The attack rate is 1.52 per 100,000 population. Dengue cases have risen by 11.5 times, compared with the same period in 2011.(![]()
![]() Reference)
Reference)
Asia:
India (Pune, Maharashtra state): Dengue in 2013: 32 cases; Deaths 2.
Philippines (Cebu city): Dengue in 2013: 115 cases.
Australia (Cairns, North Queensland). Dengue in 2013: Whitfield area 30 cases; Mount Sheridan 7 cases; Dengue virus type 1.
France: more than 23,000 cases of measles including 6 deaths were reported in France between 1 Jan 2008 and 16 Jan 2013, according to data released by l’Institut de Veille Sanitaire (The Institute of Public Health). The greatest incidence is affecting southwest area. Last year 2012, 859 cases were reported with 3 cases of encephalitis and 32 cases of severe pneumonia.
England (North-East): almost 50 cases of measles were confirmed in recent months (since Sptember 2012). The Health Protection Agency urged adults to check whether they and their children are protected with 2 doses of MMR vaccine. The majority of cases are in unvaccinated school children and young adults with >50% of the cases aged between 10 and 30 years. Most of these cases could have been avoided if people had been up to date with MMR vaccination. The HPA is advising people with symptoms to stay away from school or work until at least 4 days after a rash has appeared.
Nigeria (Kebbi): Nigeria is one of the countries with highest number of unvaccinated children against measles. WHO stated 1.7 million Nigerian children did not receive the 1st dose of the MMR vaccine in 2011.
Pakistan (Punjab):
- 23 cases of measles in Rawalpindi. According to the WHO, more than 300 children have died from measles in Pakistan in 2012, a 5-fold increase from 2011. This situation is further evidence of the crisis in medical care in Pakistan. Rawalpindi is a city in the Pothohar region of Pakistan near the country’s capital city of Islamabad, in the province of Punjab. Rawalpindi is the 4th largest city in Pakistan after Karachi, Lahore and Faisalabad.
- 92 cases of measles have been confirmed in Lahore, according to the Health Department. A 10-year-old died of measles at Mayo Hospital’s paediatric ward on Wednesday 23 Jan 2013.
- 40 cases of measles have been reported in Multan. Vaccination teams had been set up to inoculate children in affected areas.
- 6 new measles patients were reported in Gujranwala on Wednesday 23 Jan 2013.
Pakistan (vaccination policy): The Health Department has decided to lower the age of 1st measles vaccination from 9 months to 6 months in areas where cases are being reported.
Brazil: The State of Sao Paulo (SP) has had no endemic circulation of measles virus since 2000. However, in 2011, there were 27 measles cases, with 18 of them occurring as 2 outbreaks in schools. Most cases (23) in SP occurred between August and December 2011. There was no record of any confirmed cases of measles in SP during 2012. On Wed 2nd Jan 2013, a suspected case of measles in a 20-year-old resident of the city of Bauru (SP state) with a history of international travel to Florida, USA in December 2012 tested positive for measles virus genotype D8 by RT-PCR and sequencing performed at Fiocruzon on the initial sample (2 Jan 2013). Measles virus genotype D8 is circulating in England and has been detected in other countries, including the USA, Canada and China. On Wed 9 Jan 2013, a traveler living in Minas Gerais, who returned on the same flight, presented with rash and fever. On Thu 10 Jan 2013, 2 family contacts who had accompanied the 1st case also became symptomatic. All cases are under investigation until the final diagnosis.
Andhra Pradesh: poor vector-control measures have led to a massive rise in malaria cases. Hyderabad recorded 51 malaria cases in December 2012 against 5 cases in the previous year. Nine cases have been reported in the last 9 days. Although November and December are months with declining mosquito-borne diseases the high numbers of this year reflect that vector control measures are not being taken care of adequately. The majority of cases are being reported from the Old City and Amberpet. Last year 2012 during the monsoon season, the government organised several anti-malaria campaigns in the city, where they highlighted how mosquito-borne diseases like malaria, dengue and chikungunya can be controlled by effective measures taken by residents.(![]() Reference)
Reference)
Goa: a few malaria cases have been reported among the local population and staff of barges anchored at the dry docks along the Zuari river at Cortalim (Goa). Health authorities have cautioned the vessels’ owners and others to maintain hygiene in the area. The hanging tyres on the sides of the barges filled with water are the perfect breeding grounds for mosquitoes, and this has led to some barge workers and locals contracting malaria.(![]() Reference)
Reference)
Of 28 cases of suspected Chikungunya cases with fever, rashes and joint pains reported in Barangay Guintarcan of Villareal, Samar, 10 were finally confirmed. The Research Institute for Tropical Medicine is also investigating 235 other cases with the same symptoms reported in Barangay Banquil, also in Villareal. The Department of Health has recorded confirmed cases of Chikungunya in Samar, Laguna, Pangasinan, Saranggani and Metro Manila. No deaths has so far been reported, but health authorities are now undertaking measures to stop its spread. There were sporadic outbreaks of Chikungunya virus infections last year (2012) in various parts of the Philippines. Chikungunya virus is doubtless endemic in the Philippines, having caused sporadic outbreaks in 1954, 1956, 1968, and 1985 to 1986, mainly in the center and south areas of the country. Since there is no commercially available vaccine, the only preventive measures are mosquito vector control and avoidance of mosquito bites. (![]() Reference)
Reference)
On 18. January 2013, the WHO reported that wild poliovirus type 1 has been found in sewage samples in 2 different districts in Cairo (Al Haggana (Nasr City) and Al Salam), Egypt (see posting from 22. Jan. 2013 below). This wild poliovirus type 1 is related to the poliovirus reported in September 2012 from northern Sindh (Pakistan), and it’s the first documented importation of wild poliovirus from Pakistan in Egypt, since this country was declared polio free in 2004. So far, no case of polio has been reported in association with this importation. Field investigation and active search for cases is ongoing in Egypt. A supplementary immunization campaign for children under 5 years of age is planned over the next months. (![]() Reference)
Reference)
A new GII.4 Norovirus strain was identified in Australia in March 2012. Named GII.4 Sydney, this emergent strain has since caused acute gastroenteritis outbreaks in multiple countries. During September–December 2012, a total of 141 (53%) of the 266 norovirus outbreaks reported to CaliciNet were caused by GII.4 Sydney that appears to have replaced the previously predominant strain, GII.4 New Orleans. Compared with other norovirus genotypes, GII.4 noroviruses have been associated with increased rates of hospitalizations and deaths during outbreaks.
Noroviruses are the leading cause of epidemic gastroenteritis, including foodborne outbreaks, in the United States. Hospitalization and mortality associated with norovirus infection occur most frequently among elderly persons, young children, and immunocompromised patients. Noroviruses belong to the family Caliciviridae and can be grouped into five genogroups (GI through GV), which are further divided into at least 34 genotypes. Human disease primarily is caused by GI and GII noroviruses, with most outbreaks caused by GII.4 strains. During the past decade, new GII.4 strains have emerged every 2–3 years, replacing previously predominant GII.4 strains.
Proper hand hygiene, environmental disinfection, and isolation of ill persons remain the mainstays of norovirus prevention and control. (![]() Reference)
Reference)
A new case of a potentially deadly strain of E. coli has been confirmed in New Brunswick, bringing the total number of people affected in the Maritimes and Ontario to 30. Laboratory results show all of the cases of E. coli O157 are linked. The source of the contamination for the shredded lettuce has not yet been determined. (![]() Reference)
Reference)
Egypt/Pakistan: Two sewage samples from Cairo were analysed and found to resemble a recently discovered strain in the Pakistani city of Sukkur. To reduce the possibility of spread of poliovirus beyond Pakistan’s borders all children under 5 years leaving the country are being vaccinated against poliovirus at the international departure lounges. Polio cases in Pakistan have risen sharply in recent years, hitting 198 in 2011, according to the WHO.
Afghanistan: Total number of WPV cases for 2012: 37. Total number of cVDPV2 cases for 2012: 4.
Nigeria: One new WPV case was reported in the past week, total number of WPV cases for 2012: 122. 2 new cases of cVDVP2 were reported in the past week. Total number of cVDPV2 cases for 2012: 8.
Pakistan: Total number of WPV cases for 2012: 58. Total number of cVDPV2 cases for 2012: 15.
Niger: In the 1st outbreak of polio in 2012 outside of an endemic country or a country with re-established poliovirus, Niger has reported a case of wild poliovirus. This is the 1st case in the country since December 2011 and is related to virus originating in Nigeria.
Bolivia: 370 Dengue confirmed cases and 1,560 Dengue suspected cases. The areas most affected are Guayaramern, Beni department, Pando department, and Santa Cruz. Caused by Dengue viruses 1,2,3.
Brazil: States affected by Dengue are: Mato Grosso do Sul state with 7,697 cases, increasing with an average of 600 cases per day; Rondonia state with 3,099 cases in 2012; and Peabiru in Parana state with 1,300 cases since June 2012.
Colombia (Antioquia department): 74 Dengue cases and increasing.
Ecuador: Santo Domingo city (Santo Domingo de los Tsachilas province) with 2,027 Dengue cases in 2012 and one DHF/serious case in 2013; Sucumbios province with more than 110 Dengue cases and 1 death associated to a Dengue suspected case.
Paraguay: 9,467 Dengue cases in last 30 days with 7 deaths associated to Dengue confirmed cases and 12 deaths associated to Dengue suspected cases.
Venezuela: 48,346 Dengue cases with Anzoategui state affected by 1,743 cases.
Cuba’s Public Health Ministry reported 51 new cholera cases in Havana on Tuesday 15th Jan 2013, and several countries are taking precautionary measures with regards to travel to and from Cuba. However, no tourists have contracted cholera since the outbreak began on 6th Jan 2013. Most of health centers in Havana instituted a policy requiring visitors to sanitize shoes by stepping in chlorine upon entering. State schools are stressing hand washing and other hygienic measures. (![]() Reference)
Reference)
Angola (Northern Uije province): Cholera cases have been increasing in over the past days. Local authorities said that this is due to heavy rains hitting the region, and advised the population to take preventive measures. (![]() Reference)
Reference)
Ghana (Ashanti Region): a cholera outbreak was started last Monday after patients were reporting with symptoms at medical establishments in the municipality. One death and more than 50 people hospitalised. Obuasi, a major mining community, is currently suffering from sanitation inadequacies resulting from the breakdown of some of the municipal assembly’s skip loaders. (![]() Reference)
Reference)
A new tick-borne infection, similar to Lyme disease, has been found in humans in Connecticut, Massachusetts, Rhode Island, New York for the 1st time. It’s carried by deer ticks, caused by a bacterium named Borrelia miyamotoi, and has the same treatment as Lyme disease. Symptoms are similar to Lyme – fever, headache, muscle ache, and fatigue. The relapsing-fever group of Borrelia, which includes B. miyamotoi, is genetically diverse and causes a disease characterized by a high temperature that cyclically remits. Borrelia hermsii is the most frequent cause of tick-borne relapsing fever in the USA. Humans typically are exposed to these ticks during an overnight stay in rodent-infested dwellings at elevations greater than 2000 feet. In the USA, a majority of the reported cases are from California and Washington. (![]() Reference)
Reference)
On 3. October 2012, the public health authorities of Portugal reported 2 autochthonous cases of dengue fever in patients residing in the Autonomous Region of Madeira. This signalled the onset of the first recorded outbreak of dengue in Madeira. As of 6. January 2013, 2.144 cases of dengue infection have been reported in Madeira and 13 European countries have reported dengue cases among travellers returning from Madeira. The presence of Aedes aegypti mosquitoes, the main vector for transmission of the virus, has been documented in Madeira since 2005. (![]()
![]() Reference)
Reference)

